|
|
||||||||||
|
||||||||||
|
||||||||||
Unsubscribe · Manage your email preferences · Privacy policy We’d love to hear from you! Send us feedback or contact us through our help center. · |
Brain disorders, stress , sleep and diseases
12 Effects of Chronic Stress on Your Brain | Be Brain Fit
Chronic stress increases the stress hormone cortisol and affects many brain functions, putting you at risk for many mood disorders and other mental issues. … free radicals. If stress causes you to losesleep, eat junk food, drink too much alcohol, or smoke cigarettes to relax, these are contributing to your free radical load.
Extent and Health Consequences of Chronic Sleep Loss and Sleep …
It is estimated that 50 to 70 million Americans chronically suffer from a disorder of sleep and wakefulness, hindering daily functioning and adversely affecting health and … Adults with chronic sleeploss report excess mental distress, depressive symptoms, anxiety, and alcohol use (Baldwin and Daugherty, 2004; Strine and …
Traumatic stress: effects on the brain – NCBI – NIH
Traumatic stressors such as early trauma can lead to posttraumatic stress disorder (PTSD), whichaffects about 8% of Americans at some time In their lives, … PTSD is characterized by specific symptoms, including intrusive thoughts, hyperarousal, flashbacks, nightmares, and sleep disturbances, changes in memory and …
11 Effects of Sleep Deprivation on Your Body – Healthline
Jun 5, 2017 – Science has linked poor slumber with all kinds of health problems, from weight gain to a weakened immune system. sleep deprivation. Your body needs sleep, just as it needs air and food to function at its best. During sleep, your body heals itself and restores its chemical balance. Your brainforges new …
Chronic Stress Can Damage Brain Structure and Connectivity …
Feb 12, 2014 – The finding suggests a key role for oligodendrocytes in long-term and perhaps permanent changes in the brain that could set the stage for later mental problems. Chronic stress decreases the number of stem cells that mature into neurons and might provide an explanation for how chronic stressalso affects …
Sleep and mental health – Harvard Health
Jul 1, 2009 – In bipolar depression, however, studies report that 23% to 78% of patients sleep excessively (hypersomnia), while others may experience insomnia or restless sleep. … Sleep problems also adversely affect mood and contribute to relapse. Anxiety disorders.
The gut-brain connection – Harvard Health
In other words, stress (or depression or other psychological factors) can affect movement and contractions of the GI tract, make inflammation worse, or perhaps make you more susceptible toinfection. In addition, research suggests that some people with functional GI disorders perceive pain more acutely than other people …
10 Surprising Effects of Lack of Sleep – WebMD
Feb 13, 2014 – Here are 10 surprising — and serious — effects of sleep loss. … Problems. Sleep disordersand chronic sleep loss can put you at risk for: … According to some estimates, 90% of people with insomnia — a sleep disorder characterized by trouble falling and staying asleep — also have another health condition.
10 Facts You Might Not Know About Sleep and Mental Health …
May 23, 2017 – Poor sleep habits have been linked to problems like: depression and anxiety, increased risk for heart disease and cancer, memory issues, reduced immune … May is Mental Health Awareness Month, and to have a better understanding of how sleep affects your mental health, check out these 10 facts: 1.
Sleep Disorders | Anxiety and Depression Association of America, ADAA
Stress or anxiety can cause a serious night without sleep, as do a variety of other problems. Insomnia is the … Anxiety causes sleeping problems, and new research suggests sleep deprivation can cause ananxiety disorder. Research also … Sleeping recharges your brain and improves your focus, concentration, and mood.
Single neurons regulate their overall action potential firing rate
Microglia cells survey synapses by engulfing them
 Microglial cells fulfill a variety of different tasks within the CNS mainly related to both immune response and maintaining homeostasis. The following are some of the major known functions carried out by these cells.[citation needed]
Microglial cells fulfill a variety of different tasks within the CNS mainly related to both immune response and maintaining homeostasis. The following are some of the major known functions carried out by these cells.[citation needed]
Scavenging
In addition to being very sensitive to small changes in their environment, each microglial cell also physically surveys its domain on a regular basis. This action is carried out in the ameboid and resting states. While moving through its set region, if the microglial cell finds any foreign material, damaged cells, apoptotic cells, neurofibrillary tangles, DNA fragments, or plaques it will activate and phagocytose the material or cell. In this manner microglial cells also act as “housekeepers”, cleaning up random cellular debris.[14] During developmental wiring of the brain, microglial cells play a large role regulating numbers of neural precursor cells and removing apoptotic neurons. There is also evidence that microglia can refine synaptic circuitry by engulfing and eliminating synapses[22]. Post development, the majority of dead or apoptotic cells are found in the cerebral cortex and the subcortical white matter. This may explain why the majority of ameboid microglial cells are found within the “fountains of microglia” in the cerebral cortex.[19]
Phagocytosis
The main role of microglia, phagocytosis, involves the engulfing of various materials. Engulfed materials generally consist of cellular debris, lipids, and apoptotic cells in the non-inflamed state, and invading virus, bacteria, or other foreign materials in the inflamed state. Once the microglial cell is “full” it stops phagocytic activity and changes into a relatively non-reactive gitter cell.[citation needed]
Extracellular signaling
A large part of microglial cell’s role in the brain is maintaining homeostasis in non-infected regions and promoting inflammation in infected or damaged tissue. Microglia accomplish this through an extremely complicated series of extracellular signaling molecules which allow them to communicate with other microglia, astrocytes, nerves, T-cells, and myeloid progenitor cells. As mentioned above the cytokine IFN-γ can be used to activate microglial cells. In addition, after becoming activated with IFN-γ, microglia also release more IFN-γ into the extracellular space. This activates more microglia and starts a cytokine induced activation cascade rapidly activating all nearby microglia. Microglia-produced TNF-α causes neural tissue to undergo apoptosis and increases inflammation. IL-8 promotes B-cell growth and differentiation, allowing it to assist microglia in fighting infection. Another cytokine, IL-1, inhibits the cytokines IL-10 and TGF-β, which downregulate antigen presentation and pro-inflammatory signaling. Additional dendritic cells and T-cells are recruited to the site of injury through the microglial production of the chemotactic molecules like MDC, IL-8, and MIP-3β. Finally, PGE2 and other prostanoids prevent chronic inflammation by inhibiting microglial pro-inflammatory response and downregulating Th1 (T-helper cell) response.[14]
Antigen presentation
As mentioned above, resident non-activated microglia act as poor antigen presenting cells due to their lack of MHC class I/II proteins. Upon activation they rapidly uptake MHC class I/II proteins and quickly become efficient antigen presenters. In some cases, microglia can also be activated by IFN-γ to present antigens, but do not function as effectively as if they had undergone uptake of MHC class I/II proteins. During inflammation, T-cells cross the blood–brain barrier thanks to specialized surface markers and then directly bind to microglia in order to receive antigens. Once they have been presented with antigens, T-cells go on to fulfill a variety of roles including pro-inflammatory recruitment, formation of immunomemories, secretion of cytotoxic materials, and direct attacks on the plasma membranes of foreign cells.[6][14]
Cytotoxicity
In addition to being able to destroy infectious organisms through cell to cell contact via phagocytosis, microglia can also release a variety of cytotoxic substances. Microglia in culture secrete large amounts of hydrogen peroxide and nitric oxide in a process known as ‘respiratory burst‘. Both of these chemicals can directly damage cells and lead to neuronal cell death. Proteases secreted by microglia catabolise specific proteins causing direct cellular damage, while cytokines like IL-1 promote demyelination of neuronal axons. Finally, microglia can injure neurons through NMDA receptor-mediated processes by secreting glutamate, aspartate and quinolinic acid. Cytotoxic secretion is aimed at destroying infected neurons, virus, and bacteria, but can also cause large amounts of collateral neural damage. As a result, chronic inflammatory response can result in large scale neural damage as the microglia ravage the brain in an attempt to destroy the invading infection.[6]
Synaptic stripping
In a phenomenon first noticed in spinal lesions by Blinzinger and Kreutzberg in 1968, post-inflammation microglia remove the branches from nerves near damaged tissue. This helps promote regrowth and remapping of damaged neural circuitry.[6]
Promotion of repair
Post-inflammation, microglia undergo several steps to promote regrowth of neural tissue. These include synaptic stripping, secretion of anti-inflammatory cytokines, recruitment of neurons and astrocytes to the damaged area, and formation of gitter cells. Without microglial cells regrowth and remapping would be considerably slower in the resident areas of the CNS and almost impossible in many of the vascular systems surrounding the brain and eyes.
Early synapse loss to Alzheimer’s disease


| Structure of a typical chemical synapse |
|---|
In the nervous system, a synapse[1] is a structure that permits a neuron (or nerve cell) to pass an electrical or chemical signal to another neuron or to the target efferent cell.
Santiago Ramón y Cajal proposed that neurons are not continuous throughout the body, yet still communicate with each other, an idea known as the neuron doctrine.[2] The word “synapse” – from the Greek synapsis (συνάψις), meaning “conjunction”, in turn from συνάπτεὶν (συν (“together”) and ἅπτειν (“to fasten”)) – was introduced in 1897 by the English neurophysiologist Charles Sherringtonin Michael Foster‘s Textbook of Physiology.[1] Sherrington struggled to find a good term that emphasized a union between two separate elements, and the actual term “synapse” was suggested by the English classical scholar Arthur Woollgar Verrall, a friend of Michael Foster.[3][4]Some authors generalize the concept of the synapse to include the communication from a neuron to any other cell type,[5] such as to a motor cell, although such non-neuronal contacts may be referred to as junctions (a historically older term).
Synapses are essential to neuronal function: neurons are cells that are specialized to pass signals to individual target cells, and synapses are the means by which they do so. At a synapse, the plasma membrane of the signal-passing neuron (the presynaptic neuron) comes into close apposition with the membrane of the target (postsynaptic) cell. Both the presynaptic and postsynaptic sites contain extensive arrays of a molecular machinery that link the two membranes together and carry out the signaling process. In many synapses, the presynaptic part is located on an axon and the postsynaptic part is located on a dendrite or soma. Astrocytes also exchange information with the synaptic neurons, responding to synaptic activity and, in turn, regulating neurotransmission.[6] Synapses (at least chemical synapses) are stabilized in position by synaptic adhesion molecules (SAMs) projecting from both the pre- and post-synaptic neuron and sticking together where they overlap; SAMs may also assist in the generation and functioning of synapses.[7]
Contents
[hide]
Chemical or electrical
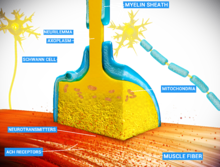
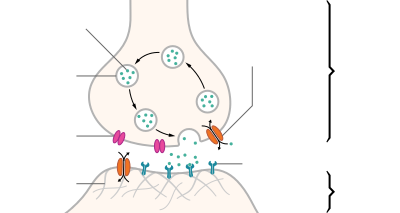
An example of chemical synapse by the release of neurotransmitters like acetylcholine or glutamic acid.
There are two fundamentally different types of synapses:
- In a chemical synapse, electrical activity in the presynaptic neuron is converted (via the activation of voltage-gated calcium channels) into the release of a chemical called a neurotransmitter that binds to receptors located in the plasma membrane of the postsynaptic cell. The neurotransmitter may initiate an electrical response or a secondary messenger pathway that may either excite or inhibit the postsynaptic neuron. Chemical synapses can be classified according to the neurotransmitter released: glutamatergic (often excitatory), GABAergic (often inhibitory), cholinergic (e.g. vertebrate neuromuscular junction), and adrenergic (releasing norepinephrine). Because of the complexity of receptor signal transduction, chemical synapses can have complex effects on the postsynaptic cell.
- In an electrical synapse, the presynaptic and postsynaptic cell membranes are connected by special channels called gap junctions or synaptic cleft that are capable of passing an electric current, causing voltage changes in the presynaptic cell to induce voltage changes in the postsynaptic cell. The main advantage of an electrical synapse is the rapid transfer of signals from one cell to the next.[8]
Synaptic communication is distinct from an ephaptic coupling, in which communication between neurons occurs via indirect electric fields.
An autapse is a chemical or electrical synapse that forms when the axon of one neuron synapses onto dendrites of the same neuron.
Types of interfaces
Synapses can be classified by the type of cellular structures serving as the pre- and post-synaptic components. The vast majority of synapses in the mammalian nervous system are classical axo-dendritic synapses (axon synapsing upon a dendrite), however, a variety of other arrangements exist. These include but are not limited to axo-axonic, dendro-dendritic, axo-secretory, somato-dendritic, dendro-somatic, and somato-somatic synapses.
The axon can synapse onto a dendrite, onto a cell body, or onto another axon or axon terminal, as well as into the bloodstream or diffusely into the adjacent nervous tissue.
Role in memory
It is widely accepted that the synapse plays a role in the formation of memory. As neurotransmitters activate receptors across the synaptic cleft, the connection between the two neurons is strengthened when both neurons are active at the same time, as a result of the receptor’s signaling mechanisms. The strength of two connected neural pathways is thought to result in the storage of information, resulting in memory. This process of synaptic strengthening is known as long-term potentiation.[9]
By altering the release of neurotransmitters, the plasticity of synapses can be controlled in the presynaptic cell. The postsynaptic cell can be regulated by altering the function and number of its receptors. Changes in postsynaptic signaling are most commonly associated with a N-methyl-d-aspartic acid receptor (NMDAR)-dependent long-term potentiation (LTP) and long-term depression (LTD) due to the influx of calcium into the post-synaptic cell, which are the most analyzed forms of plasticity at excitatory synapses.[10]
Study models
For technical reasons, synaptic structure and function have been historically studied at unusually large model synapses, for example:
- Squid giant synapse
- Neuromuscular junction (NMJ), a cholinergic synapse in vertebrates, glutamatergic in insects
- Ciliary calyx in the ciliary ganglion of chicks[11]
- Calyx of Held in the brainstem
- Ribbon synapse in the retina
- Schaffer collateral synapse in the hippocampus
Synaptic polarization
The function of neurons depends upon cell polarity. The distinctive structure of nerve cells allows action potentials to travel directionally (from dendrites to cell body down the axon), and for these signals to then be received and carried on by post-synaptic neurons or received by effector cells. Nerve cells have long been used as models for cellular polarization, and of particular interest are the mechanisms underlying the polarized localization of synaptic molecules. PIP2 signaling regulated by IMPase plays an integral role in synaptic polarity.
Phosphoinositides (PIP, PIP2, and PIP3) are molecules that have been shown to affect neuronal polarity.[12] A gene (ttx-7) was identified in Caenorhabditis elegans that encodes myo-inositol monophosphatase (IMPase), an enzyme that produces inositol by dephosphorylating inositol phosphate. Organisms with mutant ttx-7 genes demonstrated behavioral and localization defects, which were rescued by expression of IMPase. This led to the conclusion that IMPase is required for the correct localization of synaptic protein components.[13][14] The egl-8 gene encodes a homolog of phospholipase Cβ (PLCβ), an enzyme that cleaves PIP2. When ttx-7 mutants also had a mutant egl-8 gene, the defects caused by the faulty ttx-7 gene were largely reversed. These results suggest that PIP2 signaling establishes polarized localization of synaptic components in living neurons.[13]
Top Bay area doctors in 2017
| Pamela J. Simms-Mackey, MD |
| Adolescent medicine, ADD/ADHD, asthma, breast-feeding |
| 5220 Claremont Ave. |
| Oakland, 510-428-3226 |
| UCSF Benioff Children’s Hospital Oakland |
| Jeffrey T. Tan, MD |
| 1720 El Camino Real, Ste. 205 |
| Burlingame, 650-259-5050 |
| Lucile Packard Children’s Hospital |
| Specialists |
| ADDICTION PSYCHIATRY |
| Steven L. Batki, MD |
| Addiction/substance abuse, opiate addiction, alcohol abuse, dual diagnosis |
| 125 Bulkley St. |
| Sausalito, 415-332-1350 |
| UCSF Medical Center |
| Lynn D. Bertram, MD |
| Addiction/substance abuse, anxiety & depression, psychotherapy, dual diagnosis-consultation |
| 23 Orinda Way, Ste. 309 |
| Orinda, 925-254-0700 |
| Barrett G. Levine, MD |
| Addiction/substance abuse, dual diagnosis |
| 969 Broadway, Floor 2 |
| Oakland, 510-251-0121 |
| Kaiser Permanente Oakland Medical Center |
| ADOLESCENT MEDICINE |
| Sara M. Buckelew, MD |
| Eating disorders, preventive medicine |
| 400 Parnassus Ave., Floor 2 |
| San Francisco, 415-353-2002 |
| UCSF Benioff Children’s Hospital San Francisco |
| Loris Y. Hwang, MD |
| Sexually transmitted diseases, adolescent gynecology, HPV–human papilloma virus |
| 400 Parnassus Ave., Floor 2 |
| San Francisco, 415-353-2002 |
| UCSF Benioff Children’s Hospital Oakland |
| Charles E. Irwin, MD |
| Preventive medicine |
| 400 Parnassus Ave., Floor 2 |
| San Francisco, 415-353-2002 |
| UCSF Benioff Children’s Hospital Oakland |
| ALLERGY & IMMUNOLOGY |
| Robert C. Bocian, MD/PhD |
| Asthma, drug allergy, food allergy, hay fever |
| 795 El Camino Real |
| Palo Alto, 650-853-2981 |
| Stanford University Hospital & Clinics |
| Anita Carmen Choy, MD |
| Allergy, asthma, food allergy |
| 211 Quarry Rd., Ste. 106, MC 5996 |
| Palo Alto, 650-322-3847 |
| El Camino Hospital |
| Kenneth Lien, MD |
| Asthma & allergy, sinusitis, food allergy |
| 20400 Lake Chabot Rd., Ste. 304 |
| Castro Valley, 510-537-0700 |
| Eden Medical Center |
| Matthew J. Lodewick, MD |
| Asthma, food allergy, vocal cord disorders |
| 2305 Camino Ramon, Ste. 225 |
| San Ramon, 925-327-1450 |
| John Muir Medical Center |
| Steven B. Machtinger, MD |
| Allergy, pediatric allergy & immunology |
| 100 S. Ellsworth Ave, Ste. 707 |
| San Mateo, 650-696-8230 |
| Mills–Peninsula Medical Center |
| Kari C. Nadeau, MD/PhD |
| Asthma, allergy, clinical trials |
| 730 Welch Rd. |
| Stanford, 650-723-0290 |
| Stanford University Hospital & Clinics |
| Bruce F. Paterson, MD |
| Asthma, allergy, hay fever |
| 2485 High School Ave., Ste. 127 |
| Concord, 925-685-3033 |
| John Muir Medical Center |
| Vivian E. Saper, MD |
| Autoimmune disease, asthma & allergy, pediatric allergy & immunology, pediatric rheumatology |
| 100 S. Ellsworth Ave, Ste. 707 |
| San Mateo, 650-696-8230 |
| Mills–Peninsula Medical Center |
| Schuman Tam, MD |
| Allergy, asthma |
| 6850 Geary Blvd. |
| San Francisco, 415-751-6800 |
| St. Mary’s Medical Center–San Francisco |
| June Y. Zhang, MD |
| Asthma, pediatric allergy & immunology, eczema, food allergy |
| 100 S. Ellsworth Ave., Ste. 208 |
| San Mateo, 650-343-4597 |
| Mills–Peninsula Medical Center |
| CARDIAC ELECTROPHYSIOLOGY |
| Nitish Badhwar, MD |
| Arrhythmias, atrial fibrillation, ventricular tachycardia ablation, catheter ablation |
| 400 Parnassus Ave., Floor 5 |
| San Francisco, 415-353-2554 |
| UCSF Medical Center |
| Sujoya Dey, MD |
| Arrhythmias, pacemakers/defibrillators, atrial fibrillation |
| 2 Bon Air Rd., Ste. 100 |
| Larkspur, 415-927-0666 |
| Marin General Hospital |
| Gregory Engel, MD |
| Arrhythmias, atrial fibrillation, nuclear cardiology |
| 2900 Whipple Ave., Ste. 205 |
| Redwood City, 650-363-5262 |
| Sequoia Hospital |
| Edward Gerstenfeld, MD |
| Arrhythmias, atrial fibrillation, ventricular tachycardia ablation, catheter ablation |
| 400 Parnassus Ave., Floor 5 |
| San Francisco, 415-353-2554 |
| UCSF Medical Center |
| Richard H. Hongo, MD |
| Arrhythmias, pacemakers/defibrillators, radiofrequency ablation, WPW syndrome |
| 2100 Webster St., Ste. 110 |
| San Francisco, 415-923-6500 |
| California Pacific Medical Center–Pacific Campus |
| Carleton T. Nibley, MD |
| Arrhythmias, pacemakers, defibrillators |
| 2700 Grant St., Ste. 319 |
| Concord, 925-674-2880 |
| John Muir Medical Center Concord |
| Alan B. Schwartz, MD |
| Arrhythmias, atrial fibrillation, defibrillators, pacemakers |
| 1501B Trousdale Dr., Floor 2 |
| Burlingame, 650-652-8600 |
| Mills–Peninsula Medical Center |
| Roger A. Winkle, MD |
| Arrhythmias, radiofrequency ablation, sudden death prevention, defibrillators |
| 1950 University Ave., Ste. 160 |
| East Palo Alto, 650-617-8100 |
| Sequoia Hospital |
| CARDIOVASCULAR DISEASE |
| David J. Anderson, MD |
| Interventional cardiology, congestive heart failure, coronary artery disease |
| 365 Hawthorne Ave., Ste. 201 |
| Oakland, 510-452-1345 |
| Alta Bates Summit Medical Center–Summit Campus |
| Teresa De Marco, MD |
| Pulmonary hypertension, transplant medicine–heart, heart failure |
| 400 Parnassus Ave. |
| San Francisco, 415-353-9088 |
| UCSF Medical Center |
| Jeffrey J. Guttas, MD |
| Preventive cardiology |
| 100 S. San Mateo Dr., Ste. 400 |
| San Mateo, 650-696-4100 |
| Mills–Peninsula Medical Center |
| Ann K. Kao, MD |
| Preventive cardiology, noninvasive cardiology |
| 2 Bon Air Rd., Ste. 100 |
| Larkspur, 415-927-0666 |
| Marin General Hospital |
| David H. Liang, MD/PhD |
| Marfan syndrome, cardiac imaging, echocardiography |
| 300 Pasteur Dr., Room H2157 |
| Stanford, 650-725-8246 |
| Stanford University Hospital & Clinics |
| Laurence H. Lief, MD |
| Congenital heart disease–adult, arrhythmias |
| 1199 Bush St., Ste. 240 |
| San Francisco, 415-567-9469 |
| California Pacific Medical Center–Pacific Campus |
| Paul L. Ludmer, MD |
| Arrhythmias, pacemakers, defibrillators |
| 365 Hawthorne Ave., Ste. 201 |
| Oakland, 510-452-1345 |
| Alta Bates Summit Medical Center–Summit Campus |
| Tania M. Nanevicz, MD |
| Heart disease in women, heart failure, cardiac imaging |
| 1501B Trousdale Ave., Floor 2 |
| Burlingame, 650-652-8600 |
| Mills–Peninsula Medical Center |
| Erik T. Price, MD |
| Noninvasive cardiology, interventional cardiology, angioplasty & stent placement, peripheral vascular disease |
| 87 Encina Ave. |
| Palo Alto, 650-853-2975 |
| Stanford University Hospital & Clinics |
| Rita F. Redberg, MD |
| Heart disease in women, preventive cardiology, noninvasive cardiology |
| 535 Mission Bay Blvd. S. |
| San Francisco, 415-353-2873 |
| UCSF Medical Center |
| Ingela Schnittger, MD |
| Coronary artery disease, echocardiography |
| 300 Pasteur Dr., Room A21 |
| Stanford, 650-723-6459 |
| Stanford University Hospital & Clinics |
| Pramodh S. Sidhu, MD |
| 5201 Norris Canyon Rd., Ste. 220 |
| San Ramon, 925-277-1900 |
| San Ramon Regional Medical Center |
| Joel Sklar, MD |
| Preventive cardiology, congestive heart failure |
| 2 Bon Air Rd., Ste. 100 |
| Larkspur, 415-927-0666 |
| Marin General Hospital |
| Peter I. Teng, MD |
| Cardiac CT angiography, preventive cardiology |
| 2250 Hayes St., Ste. 204 |
| San Francisco, 415-933-9100 |
| St. Mary’s Medical Center–San Francisco |
| David A. Vaughan, MD |
| 1899 Sullivan Ave., Ste. 207 |
| Daly City, 650-992-0463 |
| Seton Medical Center–Daly City |
| Jonathan G. Zaroff, MD |
| Preventive cardiology, stress management |
| 2200 O’Farrell St., Floor 4 |
| San Francisco, 415-833-2616 |
| Kaiser Permanente San Francisco Medical Center |
| CHILD & ADOLESCENT PSYCHIATRY |
| Jennifer L. Derenne, MD |
| Eating disorders, anxiety disorders, mood disorders |
| 401 Quarry Rd. |
| Stanford, 650-723-5511 |
| Lucile Packard Children’s Hospital |
| Glen R. Elliott, MD/PhD |
| Psychopharmacology, ADD/ADHD, autism spectrum disorders, bipolar/mood disorders |
| 650 Clark Way |
| Palo Alto, 650-688-3649 |
| Robert Lee Hendren, DO |
| Autism spectrum disorders, ADD/ADHD, neurodevelopmental disabilities, pervasive development disorders |
| 401 Parnassus Ave. |
| San Francisco, 415-502-3500 |
| Langley Porter Psychiatric Hospital & Clinics |
| Bennett L. Leventhal, MD |
| Autism spectrum disorders, ADD/ADHD, psychopharmacology |
| 401 Parnassus Ave. |
| San Francisco, 415-502-1924 |
| UCSF Medical Center |
| Robert A. Root, MD |
| Anxiety disorders, ADD/ADHD, mood disorders |
| 2323 Sacramento St., Ste. 214 |
| San Francisco, 415-600-3636 |
| California Pacific Medical Center–Pacific Campus |
| Marc I. Schwartz, MD |
| Behavioral disorders, anxiety disorders |
| 350 Bon Air Rd., Ste. 210 |
| Greenbrae, 415-461-8812 |
| Margo L. Thienemann, MD |
| Anxiety disorders |
| 900 Welch Rd., Ste. 207 |
| Palo Alto, 650-324-3241 |
| Lucile Packard Children’s Hospital |
| CHILD NEUROLOGY |
| Daniel C. Birnbaum, MD |
| Epilepsy, cerebral palsy, Tourette’s syndrome, headache |
| 747 52nd St., Floor 1 |
| Oakland, 510-428-3590 |
| UCSF Benioff Children’s Hospital Oakland |
| Sarah R. Cheyette, MD |
| ADD/ADHD, autism spectrum disorders, headache, seizure disorders |
| 301 Industrial Rd. |
| San Carlos, 650-596-4000 |
| Paul G. Fisher, MD |
| Neuro-oncology, brain tumors |
| 730 Welch Rd., Ste. 306 |
| Palo Alto, 650-723-0993 |
| Lucile Packard Children’s Hospital |
| Audrey E. Foster-Barber, MD/PhD |
| Neurocutaneous disorders, seizure disorders, palliative care, headache |
| 1825 4th St., 5th Floor, 5A |
| San Francisco, 415-353-7596 |
| UCSF Benioff Children’s Hospital San Francisco |
| Edward (Ted) J. Guarino, MD |
| Epilepsy, electroencephalography (EEG) |
| 2450 Samaritan Dr., Ste. 2 |
| San Jose, 408-356-4777 |
| Good Samaritan Hospital |
| Robin J. Shanahan, MD |
| 747 52nd St. |
| Oakland, 510-428-3590 |
| UCSF Benioff Children’s Hospital Oakland |
| Elliott Sherr, MD/PhD |
| Neurogenetics, autism spectrum disorders, epilepsy |
| 1825 4th St., Floor 5 |
| San Francisco, 415-353-2525 |
| UCSF Benioff Children’s Hospital San Francisco |
| CLINICAL GENETICS |
| Emily Chen, MD/PhD |
| Down syndrome, skeletal dysplasia, dysmorphology |
| 2350 Geary Blvd., Floor 3 |
| San Francisco, 415-833-2998 |
| Kaiser Permanente San Francisco Medical Center |
| Gregory M. Enns, MD |
| Inherited metabolic disorders, mitochondrial disorders |
| 730 Welch Rd., Ste. 2A |
| Palo Alto, 650-721-5804 |
| Lucile Packard Children’s Hospital |
| Louanne Hudgins, MD |
| Prenatal diagnosis |
| 730 Welch Rd., Ste. 2A |
| Palo Alto, 650-721-5804 |
| Lucile Packard Children’s Hospital |
| David A. Stevenson, MD |
| Neurofibromatosis, hereditary hemorrhagic telangiectasia, vascular malformations, Prader-Willi syndrome |
| 730 Welch Rd., Ste. 2A |
| Palo Alto, 650-721-5804 |
| Lucile Packard Children’s Hospital |
| COLON & RECTAL SURGERY |
| Michael E. Abel, MD |
| Colon & rectal cancer, minimally invasive surgery, anorectal disorders, incontinence/pelvic floor disorders |
| 3838 California St., Ste. 616 |
| San Francisco, 415-668-0411 |
| California Pacific Medical Center–Pacific Campus |
| Mark B. Bazalgette, MD |
| Colonoscopy/polypectomy, inflammatory bowel disease, colon & rectal cancer & surgery, hemorrhoids |
| 5 Bon Air Rd., Ste. 101 |
| Larkspur, 415-924-2515 |
| Marin General Hospital |
| Emily V. Finlayson, MD |
| Colon & rectal cancer, Crohn’s disease, ulcerative colitis, minimally invasive surgery |
| 1825 4th St., Floor 4 |
| San Francisco, 415-885-3606 |
| UCSF Medical Center |
| Michael M. Gottlieb, MD |
| Colon & rectal cancer, hemorrhoids, inflammatory bowel disease/Crohn’s, laparoscopic surgery |
| 1320 El Capitan Dr., Ste. 440 |
| Danville, 925-277-1117 |
| San Ramon Regional Medical Center |
| Samuel C. Oommen, MD |
| Colon & rectal cancer, gastrointestinal cancer, laparoscopic surgery, robotic surgery |
| 365 Lennon Ln., Ste. 290 |
| Walnut Creek, 925-274-9000 |
| John Muir Medical Center |
| Andrew A. Shelton, MD |
| Colon & rectal cancer, gastrointestinal cancer, inflammatory bowel disease/Crohn’s, minimally invasive surgery |
| 875 Blake Wilbur Dr., Clinic B |
| Stanford, 650-498-6000 |
| Stanford University Hospital & Clinics |
| Jeffrey A. Sternberg, MD |
| Colon & rectal cancer, minimally invasive surgery, Pilonidal disease, inflammatory bowel disease/Crohn’s |
| 3838 California St., Ste. 616 |
| San Francisco, 415-668-0411 |
| California Pacific Medical Center–Pacific Campus |
| Madhulika G. Varma, MD |
| Colon & rectal cancer, anal cancer, inflammatory bowel disease/Crohn’s, pelvic floor disorders |
| 1825 4th St., Floor 4 |
| San Francisco, 415-885-3606 |
| UCSF Medical Center |
| Mark L. Welton, MD |
| Ulcerative colitis, Crohn’s disease, colon & rectal cancer, anal cancer |
| 875 Blake Wilbur Dr., Clinic B |
| Stanford, 650-498-6000 |
| Stanford University Hospital & Clinics |
| Laurence F. Yee, MD |
| Colon & rectal cancer, laparoscopic surgery, robotic surgery, gastrointestinal surgery |
| 2100 Webster Ave., Ste. 520 |
| San Francisco, 415-923-3020 |
| California Pacific Medical Center–Pacific Campus |
| DERMATOLOGY |
| Edward V. Becker, MD |
| Cosmetic dermatology, hair & nail disorders, aging skin, medical dermatology |
| 2255 Ygnacio Valley Rd., Ste. B1 |
| Walnut Creek, 925-945-7005 |
| John Muir Medical Center |
| Timothy G. Berger, MD |
| Autoimmune disease, blistering diseases, viral infections, pemphigus |
| 1701 Divisadero St., Floor 3. |
| San Francisco, 415-353-7800 |
| UCSF–Mount Zion Medical Center |
| Stephen L. Dalton, MD/PhD |
| Cosmetic dermatology, dermatologic surgery, medical dermatology |
| 867 Diablo Ave. |
| Novato, 415-892-0754 |
| Novato Community Hospital |
| Kathy A. Fields, MD |
| Cosmetic dermatology, acne, skin cancer |
| 2100 Webster St., Ste. 505 |
| San Francisco, 415-923-3377 |
| California Pacific Medical Center–Pacific Campus |
| Ilona J. Frieden, MD |
| Pediatric dermatology, hemangiomas/birthmarks, skin laser surgery–resurfacing, vascular malformations |
| 1701 Divisadero St., Floor 3 |
| San Francisco, 415-353-7800 |
| UCSF Benioff Children’s Hospital San Francisco |
| Richard G. Glogau, MD |
| Cosmetic dermatology, aging skin, dermatologic surgery, Mohs surgery |
| 350 Parnassus Ave., Ste. 400 |
| San Francisco, 415-564-1261 |
| UCSF Medical Center |
| Roy C. Grekin, MD |
| Skin cancer, Mohs surgery, skin laser surgery–resurfacing, cosmetic dermatology |
| 1701 Divisadero St., Floor 3 |
| San Francisco, 415-353-7878 |
| UCSF–Mount Zion Medical Center |
| Youn Hee Kim, MD |
| Cutaneous lymphoma, mycosis fungoides |
| 875 Blake Wilbur Dr., Clinic A |
| Stanford, 650-498-6000 |
| Stanford University Hospital & Clinics |
| Vic A. Narurkar, MD |
| Cosmetic dermatology, skin laser surgery–resurfacing, Botox therapy, facial rejuvenation |
| 2100 Webster St., Ste. 505 |
| San Francisco, 415-923-3377 |
| California Pacific Medical Center–Pacific Campus |
| Isaac M. Neuhaus, MD |
| Skin cancer, Mohs surgery, reconstructive surgery–skin, skin laser surgery–resurfacing |
| 1701 Divisadero St., Floor 3 |
| San Francisco, 415-353-7878 |
| UCSF–Mount Zion Medical Center |
| Jon C. Starr, MD |
| Skin cancer, Mohs surgery |
| 321 Middlefield Rd., Ste. 245 |
| Menlo Park, 650-326-7222 |
| Stanford University Hospital & Clinics |
| Susan M. Swetter, MD |
| Melanoma, skin cancer, pigmented lesions |
| 900 Blake Wilbur Dr., Room W3045 |
| Stanford, 650-498-6000 |
| Stanford University Hospital & Clinics |
| Maria L. Wei, MD/PhD |
| Melanoma, pigmented lesions, melanoma risk assessment, melanoma genetics |
| 1701 Divisadero St., Floor 3 |
| San Francisco, 415-353-7800 |
| UCSF–Mount Zion Medical Center |
| DEVELOPMENTAL-BEHAVIORAL PEDIATRICS |
| Brad D. Berman, MD |
| Neurodevelopmental disabilities, autism spectrum disorders, ADD/ADHD |
| 1801 Oakland Blvd., Ste. 340 |
| Walnut Creek, 925-279-3480 |
| UCSF Medical Center |
| Heidi M. Feldman, MD/PhD |
| Developmental & behavioral disorders, autism spectrum disorders, neurodevelopmental disabilities |
| 730 Welch Rd. |
| Palo Alto, 650-725-8995 |
| Stanford University Hospital & Clinics |
| Damon R. Korb, MD |
| Developmental & behavioral disorders, neurodevelopmental disabilities, autism spectrum disorders |
| 15951 Los Gatos Blvd., Ste. 6 |
| Los Gatos, 408-358-1853 |
| DIAGNOSTIC RADIOLOGY |
| Harriet B. Borofsky, MD |
| Breast imaging, breast cancer |
| 100 S. San Mateo Dr. |
| San Mateo, 650-696-4494 |
| Mills–Peninsula Medical Center |
| Michael P. Federle, MD |
| Abdominal imaging, CT body scan |
| 300 Pasteur Dr. |
| Stanford, 650-723-6855 |
| Stanford University Hospital & Clinics |
| Beth C. Kleiner, MD |
| Ultrasound |
| 101 S. San Mateo Dr., Ste. 201 |
| San Mateo, 650-343-1655 |
| Mills–Peninsula Medical Center |
| Bernice S. Law, MD |
| Pediatric radiology, fetal MRI, CT scan, trauma radiology |
| 3700 California St. |
| San Francisco, 415-750-6025 |
| California Pacific Medical Center–California Campus |
| Susan C. Marks, MD |
| Breast imaging |
| 101 S. San Mateo Dr., Ste. 201 |
| San Mateo, 650-343-1655 |
| Mills–Peninsula Medical Center |
| Dennis S. Orwig, MD |
| 250 Bon Air Rd. |
| Greenbrae, 415-925-7080 |
| Marin General Hospital |
| Lynne S. Steinbach, MD |
| Musculoskeletal imaging, MRI, sports medicine radiology |
| 505 Parnassus Ave., Floor 3 |
| San Francisco, 415-353-2573 |
| UCSF Medical Center |
| Benjamin M. Yeh, MD |
| Abdominal imaging, liver tumors, genitourinary radiology |
| 505 Parnassus Ave. |
| San Francisco, 415-353-1821 |
| UCSF Medical Center |
| Ronald J. Zagoria, MD |
| Abdominal imaging, genitourinary radiology, interventional radiology, prostate cancer |
| 505 Parnassus Ave. |
| San Francisco, 415-353-1821 |
| UCSF Medical Center |
| ENDOCRINOLOGY, DIABETES & METABOLISM |
| Karen E. Earle, MD |
| Diabetes, thyroid disorders, pituitary disorders, adrenal disorders |
| 1375 Sutter St., Ste. 208 |
| San Francisco, 415-600-0110 |
| California Pacific Medical Center–Pacific Campus |
| Paul A. Fitzgerald, MD |
| Diabetes, hypogonadism, thyroid disorders, pheochromocytoma |
| 350 Parnassus Ave., Ste. 710 |
| San Francisco, 415-665-1136 |
| UCSF Medical Center |
| Linda M. Gaudiani, MD |
| Diabetes, osteoporosis |
| 900 S. Eliseo Dr., Ste. 201 |
| Greenbrae, 415-461-1780 |
| Marin General Hospital |
| Laurence Katznelson, MD |
| Pituitary disorders, acromegaly, Cushing’s syndrome, neuroendocrine tumors |
| 213 Quarry Rd., Floor 3 |
| Palo Alto, 650-723-6969 |
| Stanford University Hospital & Clinics |
| Beatty H. Ramsay, MD |
| Diabetes |
| 100 S. Ellsworth Ave., Ste. 700 |
| San Mateo, 650-347-0063 |
| Mills–Peninsula Medical Center |
| Robert J. Rushakoff, MD |
| Diabetes |
| 1600 Divisadero St., Ste. C431 |
| San Francisco, 415-885-3868 |
| UCSF–Mount Zion Medical Center |
| Peter M. Sklarin, MD |
| Thyroid cancer, thyroid ultrasound, parathyroid disorders, osteoporosis |
| 1300 Crane St., Floor 2 |
| Menlo Park, 650-498-6652 |
| Stanford University Hospital & Clinics |
| Kenneth Alois Woeber, MD |
| Thyroid disorders |
| 2200 Post St., Ste. C432 |
| San Francisco, 415-885-7574 |
| UCSF Medical Center |
| GASTROENTEROLOGY |
| Aijaz Ahmed, MD |
| Transplant medicine–liver, liver disease |
| 300 Pasteur Dr., Room A160 |
| Stanford, 650-498-7878 |
| Stanford University Hospital & Clinics |
| Richard Auld, MD |
| Inflammatory bowel disease, ulcerative colitis/Crohn’s, complementary medicine |
| 34 Mark West Springs Rd., Ste. 200 |
| Santa Rosa, 707-541-7900 |
| Sutter Santa Rosa Regional Hospital |
| Subhas Banerjee, MD |
| Endoscopic therapies, pancreatic/biliary endoscopy (ERCP) |
| 900 Blake Wilbur Dr. |
| Palo Alto, 650-736-5555 |
| Stanford University Hospital & Clinics |
| Douglas A. Corley, MD/PhD |
| Gastrointestinal cancer, colon cancer screening, endoscopy & colonoscopy, pancreatic/biliary endoscopy (ERCP) |
| 2350 Geary Blvd., Floor 2 |
| San Francisco, 415-833-4579 |
| Kaiser Permanente San Francisco Medical Center |
| Timothy J. Davern, MD |
| Liver failure, transplant medicine–liver |
| 2340 Clay St., Floor 3 |
| San Francisco, 415-600-1020 |
| California Pacific Medical Center–Pacific Campus |
| Mark H. Kogan, MD |
| Colon cancer screening, inflammatory bowel disease, endoscopy |
| 2089 Vale Rd., Ste. 33 |
| San Pablo, 510-234-5012 |
| Alta Bates Summit Medical Center–Alta Bates Campus |
| Annette Y. Kwon, MD |
| Inflammatory bowel disease |
| 2100 Webster St., Ste. 423 |
| San Francisco, 415-923-6565 |
| California Pacific Medical Center–Pacific Campus |
| James W. Ostroff, MD |
| Endoscopic therapies, pancreatic disease, pancreatic/biliary endoscopy (ERCP), liver disease |
| 350 Parnassus Ave., Ste. 410 |
| San Francisco, 415-502-2112 |
| UCSF Medical Center |
| Jonathan P. Terdiman, MD |
| Inflammatory bowel disease, colon & rectal cancer detection, cancer risk assessment, hereditary cancer |
| 1701 Divisadero St., Ste. 120 |
| San Francisco, 415-502-4444 |
| UCSF–Mount Zion Medical Center |
| James D. Torosis, MD |
| Liver disease, endoscopy |
| 2900 Whipple Ave., Ste. 245 |
| Redwood City, 650-365-3700 |
| Sequoia Hospital |
| Michael S. Verhille, MD |
| Colon cancer screening, gastroesophageal reflux disease (GERD), Inflammatory bowel disease |
| 3838 California St., Ste. 416 |
| San Francisco, 415-387-8800 |
| California Pacific Medical Center–California Campus |
| GERIATRIC PSYCHIATRY |
| Mary G. De May, MD |
| Alzheimer’s disease, dementia, memory disorders |
| 1500 Owens St., Ste. 320 |
| San Francisco, 415-353-8769 |
| UCSF Medical Center |
| GYNECOLOGIC ONCOLOGY |
| John CK Chan, MD |
| Ovarian cancer, gene therapy, clinical trials, pelvic tumors |
| 3838 California St., Ste. 410 |
| San Francisco, 415-751-1847 |
| California Pacific Medical Center–California Campus |
| Lee-May Chen, MD |
| Gynecologic cancers, ovarian cancer, cancer genetics |
| 1825 4th St., Floor 4 |
| San Francisco, 415-353-9600 |
| UCSF Medical Center |
| Albert L. Pisani, MD |
| Gynecologic cancers, pelvic reconstruction, laparoscopic surgery, robotic surgery |
| 2490 Hospital Dr., Ste. 111 |
| Mountain View, 650-934-7520 |
| Mills–Peninsula Medical Center |
| Jeffrey L. Stern, MD |
| Gynecologic cancers, laparoscopic surgery |
| 2001 Dwight Way |
| Berkeley, 510-204-5770 |
| Alta Bates Summit Medical Center–Alta Bates Campus |
| Stefanie M. Ueda, MD |
| Gynecologic cancers, ovarian cancer, robotic surgery |
| 1825 4th St., Floor 4 |
| San Francisco, 415-353-9600 |
| UCSF Medical Center |
| HAND SURGERY |
| Daniel P. Birkbeck, MD |
| Hand & wrist surgery, elbow surgery, arthritis, trauma |
| 3273 Claremont Way, Ste. 100 |
| Napa, 707-254-7117 |
| Queen of the Valley Hospital |
| James Chang, MD |
| Hand & upper extremity surgery, reconstructive surgery, pediatric hand surgery, peripheral nerve surgery |
| 450 Broadway St., Floor 2 |
| Redwood City, 650-723-5256 |
| Stanford University Hospital & Clinics |
| Michael W. Grafe, MD |
| Hand & upper extremity surgery, trauma, shoulder surgery, elbow surgery |
| 208 Concourse Blvd., Ste. 1 |
| Santa Rosa, 707-544-3400 |
| Santa Rosa Memorial Hospital |
| Scott L. Hansen, MD |
| Hand & microvascular surgery, reconstructive microvascular surgery, breast reconstruction, wound healing/care |
| 350 Parnassus Ave., Ste. 509 |
| San Francisco, 415-353-4217 |
| UCSF Medical Center |
| Amy L. Ladd, MD |
| Hand & upper extremity surgery, hand injuries–pediatric |
| 450 Broadway St., Floor 2 |
| Redwood City, 650-723-5256 |
| Stanford University Hospital & Clinics |
| Lisa L. Lattanza, MD |
| Congenital hand deformities, elbow reconstruction, arthritis, fractures |
| 1500 Owens St. |
| San Francisco, 415-353-2808 |
| UCSF Medical Center |
| Kendrick E. Lee, MD |
| Microsurgery, reconstructive surgery, peripheral nerve surgery, hand injuries–pediatric |
| 3010 Colby St., Ste. 118 |
| Berkeley, 510-238-1200 |
| Alta Bates Summit Medical Center–Alta Bates Campus |
| David L. Nelson, MD |
| Arthritis, carpal tunnel syndrome, fractures, wrist/hand injuries |
| 1363 S Eliseo Dr., Ste. B |
| Greenbrae, 415-925-0501 |
| Marin General Hospital |
| Andrew J. Stein, MD |
| Hand & wrist surgery, elbow surgery, shoulder surgery |
| 13690 E. 14th St., Ste. 200 |
| San Leandro, 510-297-0550 |
| San Leandro Hospital |
| Jeffrey Yao, MD/PhD |
| Elbow reconstruction, hand & upper extremity surgery, arthroscopic wrist surgery |
| 450 Broadway St., Ste. A26 |
| Redwood City, 650-723-5256 |
| Stanford University Hospital & Clinics |
| Rebecca S. Yu, MD |
| Hand & upper extremity surgery, nerve & tendon reconstruction, arthroscopic wrist surgery, fractures |
| 3000 Colby St., Ste. 304 |
| Berkeley, 510-540-6800 |
| Alta Bates Summit Medical Center–Alta Bates Campus |
| HEMATOLOGY |
| Lloyd E. Damon, MD |
| Leukemia & lymphoma, bone marrow & stem cell transplant |
| 400 Parnassus Ave., Floor 4 |
| San Francisco, 415-353-2421 |
| UCSF Medical Center |
| Lawrence D. Kaplan, MD |
| Lymphoma, AIDS-related cancers |
| 400 Parnassus Ave., Floor 4 |
| San Francisco, 415-353-2421 |
| UCSF Medical Center |
| Thomas G. Martin, MD |
| Multiple myeloma, leukemia, bone marrow transplant |
| 400 Parnassus Ave., Floor 4 |
| San Francisco, 415-353-2421 |
| UCSF Medical Center |
| Robert S. Negrin, MD |
| Bone marrow transplant, hematologic malignancies |
| 269 W. Campus Dr., Room 2205 |
| Stanford, 650-498-6000 |
| Stanford University Hospital & Clinics |
| INFECTIOUS DISEASE |
| Jorge R. Bernett, MD |
| AIDS/HIV, hepatitis C |
| 365 Lennon Ln., Ste. 200 |
| Walnut Creek, 925-947-2334 |
| Sutter Delta Medical Center |
| Kim S. Erlich, MD |
| Sexually transmitted diseases, HIV/AIDS |
| 1501 Trousdale Dr. |
| Burlingame, 650-696-5777 |
| Mills–Peninsula Medical Center |
| Jesus R. Gatpolintan, MD |
| HIV/AIDS, sexually transmitted diseases, tick-borne diseases |
| 1375 Sutter St., Ste. 308 |
| San Francisco, 415-600-0140 |
| California Pacific Medical Center–California Campus |
| Shelley M. Gordon, MD/PhD |
| HIV/AIDS |
| 2100 Webster St., Ste. 400 |
| San Francisco, 415-923-3883 |
| California Pacific Medical Center–Pacific Campus |
| Carol A. Kemper, MD |
| HIV |
| 701 E. El Camino Real, Floor 3 |
| Mountain View, 650-934-7599 |
| Santa Clara Valley Medical Center |
| Joel M. Palefsky, MD |
| HPV–human papilloma virus, AIDS/HIV, AIDS-related cancers, Epstein-Barr virus |
| 1701 Divisadero St., Ste. 480 |
| San Francisco, 415-353-7100 |
| UCSF–Mount Zion Medical Center |
| Scott A. Weisenberg, MD |
| Travel medicine, tropical diseases |
| 350 30th St., Ste. 320 |
| Oakland, 510-465-6700 |
| Alta Bates Summit Medical Center–Summit Campus |
| Lory D. Wiviott, MD |
| HIV/AIDS |
| 2100 Webster St., Ste. 400 |
| San Francisco, 415-923-3883 |
| California Pacific Medical Center–Pacific Campus |
| INTERVENTIONAL CARDIOLOGY |
| John H. Chiu, MD |
| Peripheral vascular disease |
| 365 Hawthorne Ave., Ste. 201 |
| Oakland, 510-452-1345 |
| Alta Bates Summit Medical Center–Summit Campus |
| Ian Christoph, MD |
| Angioplasty & stent placement, cardiac catheterization, nuclear cardiology, coronary artery disease |
| 1501B Trousdale Dr., Floor 2 |
| Burlingame, 650-652-8600 |
| Mills–Peninsula Medical Center |
| William F. Fearon, MD |
| Coronary artery disease, percutaneous coronary intervention, aortic valve replacement |
| 300 Pasteur Dr., Room A31 |
| Stanford, 650-725-2621 |
| Stanford University Hospital & Clinics |
| Eric L. Johnson, MD |
| Peripheral vascular disease, carotid artery stent placement |
| 365 Hawthorne Ave., Ste. 201 |
| Oakland, 510-452-1345 |
| Alta Bates Summit Medical Center–Summit Campus |
| Sergio M. Manubens, MD |
| Cardiac catheterization |
| 3443 Villa Ln., Ste. 2 |
| Napa, 707-253-8280 |
| Queen of the Valley Hospital |
| Stephen E. Pope, MD |
| Angiography & stent placement, coronary artery disease, cardiac catheterization |
| 1501B Trousdale Dr., Floor 2 |
| Burlingame, 650-652-8600 |
| Mills–Peninsula Medical Center |
| Robert T. Sperling, MD |
| Percutaneous coronary intervention, peripheral vascular disease |
| 2 Bon Air Rd., Ste. 100 |
| Larkspur, 415-927-0666 |
| Marin General Hospital |
| Frederick S. Watson, MD |
| 100 S. San Mateo Dr., Ste. 400 |
| San Mateo, 650-696-4100 |
| Mills–Peninsula Medical Center |
| Alan C. Yeung, MD |
| Angioplasty, coronary artery disease, aortic valve replacement |
| 300 Pasteur Dr., Room A31 |
| Stanford, 650-725-2621 |
| Stanford University Hospital & Clinics |
| MATERNAL & FETAL MEDICINE |
| Maurice L. Druzin, MD |
| Pregnancy–high risk, prenatal diagnosis |
| 770 Welch Rd., Ste. 201 |
| Palo Alto, 650-498-4069 |
| Lucile Packard Children’s Hospital |
| Bonnie K. Dwyer, MD |
| Pregnancy loss, prenatal diagnosis, heart disease in pregnancy, hypertension in pregnancy |
| 2485 Hospital Dr., Ste. 231 |
| Mountain View, 650-404-8210 |
| El Camino Hospital |
| Stuart M. Lovett, MD |
| Pregnancy–high risk |
| 350 30th St., Ste. 205 |
| Oakland, 510-869-8425 |
| Alta Bates Summit Medical Center–Summit Campus |
| David N. Marinoff, MD |
| Pregnancy–high risk, diabetes in pregnancy |
| 350 30th St., Ste. 208 |
| Oakland, 510-444-0790 |
| UCSF Benioff Children’s Hospital Oakland |
| Mary E. Norton, MD |
| Prenatal diagnosis, fetal ultrasound, reproductive genetics, genetic disorders |
| 1825 4th St., Floor 3 |
| San Francisco, 415-476-4080 |
| UCSF Medical Center |
| Carl Otto, MD |
| Pregnancy–high risk, pregnancy after age 35, fetal therapy |
| 3700 California St., Ste. 4360 |
| San Francisco, 415-600-6400 |
| California Pacific Medical Center–California Campus |
| Patricia A. Robertson, MD |
| Pregnancy–high risk, prematurity prevention, premature labor |
| 1825 4th St., Floor 3 |
| San Francisco, 415-353-2566 |
| UCSF Medical Center |
| MEDICAL ONCOLOGY |
| Donald I. Abrams, MD |
| Integrative medicine, complementary Medicine, AIDS-related cancers |
| 1545 Divisadero St., Floor 4 |
| San Francisco, 415-353-7700 |
| UCSF–Mount Zion Medical Center |
| Ranjana H. Advani, MD |
| Hodgkin’s lymphoma, lymphoma, non-Hodgkin’s, clinical trials |
| 875 Blake Wilbur Dr., Clinic C |
| Stanford, 650-498-6000 |
| Stanford University Hospital & Clinics |
| Emily K. Bergsland, MD |
| Gastrointestinal cancer, colon & rectal cancer, neuroendocrine tumors |
| 1825 4th St., Floor 4 |
| San Francisco, 415-353-9888 |
| UCSF Medical Center |
| Douglas W. Blayney, MD |
| Breast cancer, cancer survivors–late effects of therapy |
| 900 Blake Wilbur Dr. |
| Palo Alto, 650-498-6004 |
| Stanford University Hospital & Clinics |
| Peter B. Brett, MD |
| Melanoma |
| 3883 Airway Dr., Ste. 220 |
| Santa Rosa, 707-521-7750 |
| Sutter Santa Rosa Regional Hospital |
| Susan M. Chang, MD |
| Brain tumors, neuro-oncology, clinical trials |
| 400 Parnassus Ave., Room A808 |
| San Francisco, 415-353-2184 |
| UCSF Medical Center |
| Adil I. Daud, MD |
| Melanoma, skin cancer, drug development, clinical trials |
| 1600 Divisadero St., Floor 3 |
| San Francisco, 415-353-9900 |
| UCSF Medical Center |
| Tyler Y. Kang, MD |
| Brain tumors, lung cancer, genitourinary cancer |
| 20400 Lake Chabot Rd., Ste. 102 |
| Castro Valley, 510-247-9227 |
| Eden Medical Center |
| Jennifer Lucas, MD |
| Breast cancer, hematologic malignancies, lymphoma |
| 1350 S. Eliseo Dr., Ste. 200 |
| Greenbrae, 415-925-5000 |
| Novato Community Hospital |
| Natalie A. Marshall, MD |
| Breast cancer, lung cancer |
| 1480 64th St., Ste. 100 |
| Emeryville, 510-629-6682 |
| Alta Bates Summit Medical Center–Alta Bates Campus |
| Daniel P. Mirda, MD |
| 1100 Trancas St., Ste. 256 |
| Napa, 707-253-7161 |
| Queen of the Valley Hospital |
| Mark D. Pegram, MD |
| Breast cancer, breast cancer–novel therapies |
| 900 Blake Wilbur Dr. |
| Palo Alto, 650-498-6004 |
| Stanford University Hospital & Clinics |
| Hope S. Rugo, MD |
| Breast cancer, complementary medicine, breast cancer–novel therapies, clinical trials |
| 1600 Divisadero St., Floor 2 |
| San Francisco, 415-353-7070 |
| UCSF–Mount Zion Medical Center |
| George W. Sledge, MD |
| Breast cancer |
| 900 Blake Wilbur Dr. |
| Palo Alto, 650-498-6004 |
| Stanford University Hospital & Clinics |
| Eric J. Small, MD |
| Prostate cancer, vaccine therapy, urologic cancer |
| 1825 4th St., Floor 4 |
| San Francisco, 415-476-4616 |
| UCSF Medical Center |
| Gregory B. Smith, MD |
| 10 Woodland Rd. |
| St Helena, 707-967-5721 |
| St. Helena Hospital |
| Melinda L. Telli, MD |
| Breast cancer, breast cancer genetics, hereditary cancer |
| 900 Blake Wilbur Dr. |
| Stanford, 650-498-6004 |
| Stanford University Hospital & Clinics |
| Margaret A. Tempero, MD |
| Pancreatic cancer, gastrointestinal cancer, pancreatic cancer–acinar cell |
| 1825 4th St., Floor 4. |
| San Francisco, 415-353-9888 |
| UCSF Medical Center |
| Alan P. Venook, MD |
| Gastrointestinal cancer, colon & rectal cancer, liver cancer |
| 1825 4th St., Floor 4 |
| San Francisco, 415-353-9888 |
| UCSF Medical Center |
| Byron E. Wilson, MD |
| 2900 Whipple Ave., Ste. 145 |
| Redwood City, 650-368-0520 |
| Sequoia Hospital |
| NEONATAL-PERINATAL MEDICINE |
| Louis P. Halamek, MD |
| 725 Welch Rd., 2 West |
| Palo Alto, 650-497-8800 |
| Lucile Packard Children’s Hospital |
| Roberta L. Keller, MD |
| Pulmonary hypertension of newborn (PPHN), lung disease in newborns, respiratory failure |
| 1975 4th St., Floor 3 |
| San Francisco, 415-353-1565 |
| UCSF Benioff Children’s Hospital San Francisco |
| NEPHROLOGY |
| Glenn M. Chertow, MD |
| Kidney disease–chronic |
| 300 Pasteur Dr., Room A11 |
| Stanford, 650-723-6961 |
| Stanford University Hospital & Clinics |
| Kerry C. Cho, MD |
| Kidney disease–chronic, amyloidosis |
| 400 Parnassus Ave. |
| San Francisco, 415-353-2507 |
| UCSF Medical Center |
| Genevieve Estilo, MD |
| 1300 S. Eliseo Dr., Ste. 104 |
| Greenbrae, 415-925-3075 |
| Marin General Hospital |
| Stephen L. Gluck, MD |
| Fluid/electrolyte balance, hypertension, kidney stones |
| 400 Parnassus Ave. |
| San Francisco, 415-353-2507 |
| UCSF Medical Center |
| Chi-Yuan Hsu, MD |
| Kidney disease–acute, kidney disease–chronic, kidney failure, hypertension |
| 400 Parnassus Ave. |
| San Francisco, 415-353-2507 |
| UCSF Medical Center |
| Kok-Tong Ling, MD |
| Kidney disease–chronic, diabetic kidney disease |
| 450 Sutter St., Ste. 935 |
| San Francisco, 415-433-7761 |
| St. Francis Memorial Hospital |
| Fred Y. Lui, MD |
| Kidney disease–chronic, hypertension, dialysis care |
| 1750 El Camino Real, Ste. 15 |
| Burlingame, 650-692-6302 |
| Mills–Peninsula Medical Center |
| Phillip Ng, MD |
| 170 Alameda de Las Pulgas, Ste. G68 |
| Redwood City, 650-327-8888 |
| Sequoia Hospital |
| John W. Riordan, MD |
| 2100 Webster St., Ste. 412 |
| San Francisco, 415-923-3815 |
| California Pacific Medical Center–Pacific Campus |
| NEUROLOGICAL SURGERY |
| Christopher P. Ames, MD |
| Spinal reconstructive surgery, spinal trauma, spinal tumors, scoliosis |
| 400 Parnassus Ave., Floor 3 |
| San Francisco, 415-353-2739 |
| UCSF Medical Center |
| Kurtis I. Auguste, MD |
| Pediatric neurosurgery, epilepsy, hydrocephalus, neuro-oncology |
| 744 52nd St., Ste. 5203 |
| Oakland, 510-428-3319 |
| UCSF Benioff Children’s Hospital Oakland |
| Mitchel S. Berger, MD |
| Brain & spinal cord tumors, stereotactic radiosurgery, neuro-oncology, epilepsy–adult & pediatric |
| 400 Parnassus Ave., Floor 8 |
| San Francisco, 415-353-7500 |
| UCSF Medical Center |
| Kenneth S. Blumenfeld, MD |
| Neuro-oncology, stereotactic radiosurgery, spinal disorders–degenerative, trauma |
| 2577 Samaritan Dr., Ste. 810 |
| San Jose, 408-358-0133 |
| Good Samaritan Hospital |
| Allen Efron, MD |
| Brain tumors, pituitary tumors, trigeminal neuralgia, cerebrovascular surgery |
| 1150 Veterans Blvd., Floor 3 |
| Redwood City, 650-299-2290 |
| Kaiser Permanente Redwood City Medical Center |
| Gerald A. Grant, MD |
| Pediatric neurosurgery, brain tumors, minimally invasive surgery, epilepsy |
| 730 Welch Rd., Floor 2 |
| Palo Alto, 650-724-4270 |
| Lucile Packard Children’s Hospital |
| Nalin Gupta, MD/PhD |
| Pediatric neurosurgery, epilepsy, congenital anomalies, brain tumors |
| 1825 4th St., Floor 5 |
| San Francisco, 415-353-2342 |
| UCSF Benioff Children’s Hospital San Francisco |
| Griffith R. Harsh, MD |
| Brain tumors, pituitary tumors, endoscopic surgery, stereotactic radiosurgery |
| 213 Quarry Rd. |
| Palo Alto, 650-723-7093 |
| Stanford University Hospital & Clinics |
| Michael T. Lawton, MD |
| Cerebrovascular surgery, skull-base tumors, arteriovenous malformations, aneurysm–cerebral |
| 400 Parnassus Ave., Floor 8 |
| San Francisco, 415-353-7500 |
| UCSF Medical Center |
| Michael W. McDermott, MD |
| Brain tumors, stereotactic radiosurgery, skull-base tumors, meningioma |
| 400 Parnassus Ave., Floor 8 |
| San Francisco, 415-353-7500 |
| UCSF Medical Center |
| Ronnie I. Mimran, MD |
| Spinal surgery, Minimally invasive spinal surgery, spinal reconstructive surgery, spinal trauma |
| 1320 El Capitan Dr., Ste. 300 |
| Danville, 925-355-9537 |
| Eden Medical Center |
| Praveen V. Mummaneni, MD |
| Spinal surgery–cervical, spinal tumors, minimally invasive spinal surgery, spinal deformity |
| 400 Parnassus Ave., Floor 3 |
| San Francisco, 415-353-2739 |
| UCSF Medical Center |
| Corey Raffel, MD/PhD |
| Pediatric neurosurgery, brain tumors, Chiari’s deformity, craniosynostosis |
| 1825 4th St., Floor 5 |
| San Francisco, 415-476-3577 |
| UCSF Medical Center |
| William F. Sheridan, MD |
| Aneurysm–cerebral, brain tumors |
| 1150 Veterans Blvd., Floor 3 |
| Redwood City, 650-299-2290 |
| Kaiser Permanente Redwood City Medical Center |
| Lawrence M. Shuer, MD |
| Brain & spinal tumors, Chiari’s deformity, syringomyelia & spinal cord diseases, epilepsy |
| 213 Quarry Rd., Floor 3 |
| Palo Alto, 650-723-6469 |
| Stanford University Hospital & Clinics |
| Gary K. Steinberg, MD/PhD |
| Aneurysm–cerebral, Moyamoya disease, arteriovenous malformations, cerebrovascular surgery |
| 213 Quarry Dr. |
| Palo Alto, 650-723-6469 |
| Stanford University Hospital & Clinics |
| Peter P. Sun, MD |
| Pediatric neurosurgery, brain tumors, endoscopic surgery, trauma |
| 744 52nd St., Ste. 5203 |
| Oakland, 510-428-3319 |
| UCSF Benioff Children’s Hospital Oakland |
| Philip V. Theodosopoulos, MD |
| Skull-base tumors, acoustic neuroma, minimally invasive surgery, pituitary tumors |
| 400 Parnassus Ave., Floor 8 |
| San Francisco, 415-353-7500 |
| UCSF Medical Center |
| Lyndell Y. Wang, MD |
| Brain tumors, hydrocephalus, aneurysm–cerebral |
| 1150 Veterans Blvd., Floor 3 |
| Redwood City, 650-299-2290 |
| Kaiser Permanente Redwood City Medical Center |
| Peter B. Weber, MD |
| Spinal surgery, epilepsy, minimally invasive spinal surgery, skull-base surgery |
| 2100 Webster St., Ste. 115 |
| San Francisco, 415-885-8628 |
| California Pacific Medical Center–Pacific Campus |
| John G. Zovickian, MD |
| Pediatric neurosurgery, spina bifida, hydrocephalus |
| 3600 Broadway, Floor 3, Room 39 |
| Oakland, 510-752-1749 |
| Kaiser Permanente Oakland Medical Center |
| NEUROLOGY |
| Gary M. Abrams, MD |
| Neuro-rehabilitation, stroke, trauma, brain injury rehabilitation |
| 400 Parnassus Ave., Floor 8 |
| San Francisco, 415-353-2273 |
| UCSF Medical Center |
| Gregory W. Albers, MD |
| Stroke, vascular neurology, cerebrovascular disease |
| 213 Quarry Rd. |
| Palo Alto, 650-723-6469 |
| Stanford University Hospital & Clinics |
| Michael S. Cohen, MD |
| Epilepsy/seizure disorders, neuromuscular disorders, stroke, dementia |
| 1501 Trousdale Dr., Floor 4 |
| Burlingame, 650-652-8350 |
| Mills–Peninsula Medical Center |
| Ilkcan Cokgor, MD/PhD |
| Neuro-oncology, headache, memory disorders, movement disorders–Botox therapy |
| 50 Red Hill Ave. |
| San Anselmo, 415-456-8180 |
| Marin General Hospital |
| John W. Engstrom, MD |
| Neuromuscular disorders, peripheral neuropathy, spinal disorders |
| 400 Parnassus Ave., Floor 8 |
| San Francisco, 415-353-2273 |
| UCSF Medical Center |
| Robert S. Fisher, MD/PhD |
| Epilepsy, seizure disorders, clinical neurophysiology |
| 213 Quarry Rd. |
| Palo Alto, 650-723-6469 |
| Stanford University Hospital & Clinics |
| Douglas S. Goodin, MD |
| Multiple sclerosis |
| 1500 Owens St., Ste. 320 |
| San Francisco, 415-353-2069 |
| UCSF Medical Center |
| Victor W. Henderson, MD |
| Alzheimer’s disease, dementia, memory disorders |
| 213 Quarry Rd., Floor 3 |
| Palo Alto, 650-723-6469 |
| Stanford University Hospital & Clinics |
| Jill L. Ostrem, MD |
| Movement disorders, Parkinson’s disease, dystonia, Botox therapy |
| 1635 Divisadero St., Ste. 520 |
| San Francisco, 415-353-2311 |
| UCSF–Mount Zion Medical Center |
| Wade S. Smith, MD/PhD |
| Stroke, stroke prevention, vascular neurology, cerebrovascular disease |
| U400 Parnassus Ave., Floor 8 |
| San Francisco, 415-353-8897 |
| UCSF Medical Center |
| Randall R. Starkey, MD |
| 365 Hawthorne Ave., Ste. 203 |
| Oakland, 510-834-5778 |
| Alta Bates Summit Medical Center–Summit Campus |
| Bradley T. Wrubel, MD |
| Neuromuscular disorders, electrodiagnosis, clinical neurophysiology, amyotrophic lateral sclerosis (ALS) |
| 2850 Telegraph Ave., Ste. 110s |
| Berkeley, 510-204-8140 |
| Alta Bates Summit Medical Center–Alta Bates Campus |
| NEURORADIOLOGY |
| William P. Dillon, MD |
| Brain tumors, head & neck radiology, cerebrovascular malformations, spinal imaging |
| 505 Parnassus Ave. |
| San Francisco, 415-353-2573 |
| UCSF Medical Center |
| Nancy J. Fischbein, MD |
| Brain tumors |
| 213 Quarry Rd. |
| Palo Alto, 650-723-6469 |
| Stanford University Hospital & Clinics |
| Randall T. Higashida, MD |
| Aneurysm–cerebral, stroke, intracranial angioplasty & stent |
| 505 Parnassus Ave., Floor 3 |
| San Francisco, 415-353-1863 |
| UCSF Medical Center |
| Max Wintermark, MD |
| Brain imaging, head & neck tumors imaging, brain & spinal imaging, stroke |
| 300 Pasteur Dr., Grant Building, Ste. S047 |
| Stanford, 650-723-7426 |
| Stanford University Hospital & Clinics |
| OBSTETRICS & GYNECOLOGY |
| Amy Meg Autry, MD |
| Minimally invasive surgery, pap smear abnormalities, endometriosis, menstrual disorders |
| 2356 Sutter St., Floor 6 |
| San Francisco, 415-885-7788 |
| UCSF–Mount Zion Medical Center |
| Secily N. Bason-Mitchell, MD |
| Pregnancy, adolescent gynecology, laparoscopic surgery, minimally invasive surgery |
| 3838 California St., Ste. 312 |
| San Francisco, 415-379-9600 |
| California Pacific Medical Center–California Campus |
| Isabell H. Beddow, MD |
| Women’s health, pregnancy, gynecologic surgery, menstrual disorders |
| 1 Baywood Ave., Ste. 5 |
| San Mateo, 650-558-0611 |
| Mills–Peninsula Medical Center |
| Sally E. Boero, MD |
| 100A Drakes Landing Rd., Ste. 225 |
| Greenbrae, 415-461-7800 |
| Marin General Hospital |
| Beatrice A. Burke, MD |
| Reproductive endocrinology, hysteroscopic surgery, minimally invasive surgery, pregnancy |
| 136 N. San Mateo Dr., Ste. 101 |
| San Mateo, 650-344-1114 |
| Mills–Peninsula Medical Center |
| Demetra L. Burrs, MD |
| Gynecology only, gay/lesbian/transgender health |
| 3200 Kearney St., Floor 2 |
| Fremont, 510-498-2182 |
| Washington Hospital |
| Sylvia J. Flores, MD |
| 100A Drakes Landing Rd., Ste. 225 |
| Greenbrae, 415-461-7800 |
| Marin General Hospital |
| David B. Galland, MD |
| Minimally invasive surgery, robotic surgery, gynecology only |
| 100A Drakes Landing Rd., Ste. 225 |
| Greenbrae, 415-461-7800 |
| Marin General Hospital |
| Mindy E. Goldman, MD |
| Breast cancer, cancer survivorship, women’s health, cancer survivorship |
| 2356 Sutter St., Floor 5 |
| San Francisco, 415-885-7788 |
| UCSF Medical Center |
| Susana G. Gonzalez, MD |
| Minimally invasive surgery, robotic surgery, menopause problems, pregnancy |
| 1100 Trancas St., Ste. 209 |
| Napa, 707-251-1850 |
| Queen of the Valley Hospital |
| Katherine T. Hsiao, MD |
| Pregnancy, gynecologic surgery |
| 3905 Sacramento St., Ste. 204 |
| San Francisco, 415-876-8500 |
| California Pacific Medical Center–California Campus |
| Leslie S. Kardos, MD |
| Gynecologic surgery, robotic surgery, laparoscopic surgery–complex, gynecology only |
| 2100 Webster St., Ste. 518 |
| San Francisco, 415-426-7859 |
| California Pacific Medical Center–Pacific Campus |
| John H. Kirk, MD |
| Robotic surgery, minimally invasive surgery, pregnancy |
| 821 S. St. Helena Hwy. |
| St Helena, 707-967-7550 |
| St. Helena Hospital |
| Lilia I. Lizano, MD |
| Women’s health, pregnancy, osteoporosis |
| 500 Alfred Nobel Dr., Ste. 200 |
| Hercules, 510-724-4435 |
| Alta Bates Summit Medical Center–Alta Bates Campus |
| Susan C. Logan, MD |
| Ultrasound |
| 500 Doyle Park Dr., Ste. 103 |
| Santa Rosa, 707-579-1102 |
| Sutter Santa Rosa Regional Hospital |
| Angela M. Pollard, MD |
| Women’s health, pregnancy |
| 700 W. Parr Ave., Ste. I |
| Los Gatos, 408-370-3100 |
| El Camino Hospital Los Gatos |
| Carrie B. Rothstein, MD |
| 321 Middlefield Rd. |
| Menlo Park, 650-498-6623 |
| Stanford University Hospital & Clinics |
| Debra Shapiro, MD |
| Pregnancy, menopause problems, preventive medicine, women’s health |
| 395 Hickey Blvd., Floor 3 |
| Daly City, 650-742-2173 |
| Kaiser Permanente South San Francisco Medical Center |
| Alison Slack, MD |
| Laparoscopic surgery, vaginal surgery, pain–pelvic, pregnancy |
| 2299 Mowry Ave., Ste. 3C |
| Fremont, 510-248-1470 |
| Washington Hospital |
| Tatiana W. Spirtos, MD |
| Minimally invasive surgery, incontinence–urinary, menopause problems, infertility |
| 2900 Whipple Ave., Ste. 135 |
| Redwood City, 650-366-5594 |
| Sequoia Hospital |
| Juan Edmundo Vargas, MD |
| Prenatal diagnosis, ultrasound, reproductive genetics, pregnancy-high risk |
| 1825 4th St., Floor 3 |
| San Francisco, 415-476-4080 |
| UCSF Medical Center |
| K. Jennifer Voss, MD |
| Minimally invasive surgery, robotic surgery |
| 100A Drakes Landing Rd., Ste. 225 |
| Greenbrae, 415-461-7800 |
| Marin General Hospital |
| OPHTHALMOLOGY |
| Steven C. Andersen, MD |
| Glaucoma, diabetic eye disease/retinopathy, macular degeneration, dry eye syndrome |
| 38707 Stivers St. |
| Fremont, 510-794-0660 |
| Washington Hospital |
| Richard A. Beller, MD |
| Glaucoma, cataract surgery, macular degeneration, retinal disorders |
| 895 Trancas St., Ste. A |
| Napa, 707-252-2020 |
| Queen of the Valley Hospital |
| Bruce H. Bern, MD |
| Cataract surgery, laser surgery, glaucoma, macular degeneration |
| 50 S. San Mateo Dr., Ste. 200 |
| San Mateo, 650-342-4595 |
| Mills–Peninsula Medical Center |
| Daniel A. Brinton, MD |
| Retinal disorders, retina/vitreous surgery, retinal detachment |
| 3300 Telegraph Ave. |
| Oakland, 510-444-1600 |
| Alta Bates Summit Medical Center–Summit Campus |
| David F. Chang, MD |
| Cataract surgery, intraocular lens replacement |
| 762 Altos Oaks Dr., Ste. 1 |
| Los Altos, 650-948-9123 |
| El Camino Hospital |
| Stewart A. Daniels, MD |
| Diabetic eye disease/retinopathy, retinal disorders |
| 122 La Casa Via, Ste. 223 |
| Walnut Creek, 925-943-6800 |
| Alta Bates Summit Medical Center–Alta Bates Campus |
| William V. Good, MD |
| Pediatric ophthalmology, eye muscle disorders, strabismus |
| 2340 Clay St., Ste. 100 |
| San Francisco, 415-202-1500 |
| California Pacific Medical Center–California Campus |
| Andrew G. Iwach, MD |
| Glaucoma, glaucoma–pediatric, laser surgery |
| 55 Stevenson St. |
| San Francisco, 415-981-2020 |
| California Pacific Medical Center–California Campus |
| Christian K. Kim, MD |
| Laser refractive surgery, corneal disease & surgery, anterior segment surgery |
| 901 E St. |
| San Rafael, 415-454-5565 |
| Novato Community Hospital |
| Scott R. Lambert, MD |
| Pediatric ophthalmology, strabismus, cataract–pediatric |
| 2452 Watson Ct. |
| Palo Alto, 650-723-6995 |
| Lucile Packard Children’s Hospital |
| Dan R. Lightfoot, MD |
| Diabetic eye disease/retinopathy, retinal disorders |
| 720 4th St. |
| Santa Rosa, 707-575-3800 |
| Sutter Santa Rosa Regional Hospital |
| Ayman Naseri, MD |
| Cataract surgery, laser refractive surgery |
| 8 Koret Way, Ste. U545 |
| San Francisco, 415-514-8200 |
| UCSF Medical Center |
| Karen W. Oxford, MD |
| Cornea transplant, cataract surgery, intraocular lens replacement, laser surgery |
| 2100 Webster St., Ste. 214 |
| San Francisco, 415-923-3007 |
| California Pacific Medical Center–Pacific Campus |
| Stuart R. Seiff, MD |
| Oculoplastic surgery, cosmetic surgery–eyes, thyroid eye disease (Graves’ disease) |
| 2100 Webster St., Ste. 214 |
| San Francisco, 415-923-3007 |
| California Pacific Medical Center–Pacific Campus |
| Gayle L. Shimokaji, MD |
| Cataract surgery, glaucoma, strabismus, oculoplastic surgery |
| 1000 S. Eliseo Dr., Ste. 203 |
| Greenbrae, 415-925-2020 |
| Marin General Hospital |
| Rona Z. Silkiss, MD |
| Oculoplastic surgery, eyelid surgery/blepharoplasty, thyroid eye disease |
| (Graves’ disease), lacrimal gland disorders |
| 711 Van Ness Ave., Ste. 570 |
| San Francisco, 415-923-3863 |
| California Pacific Medical Center–Pacific Campus |
| Allen Z. Verne, MD |
| Retinal disorders, diabetic eye disease/retinopathy, trauma |
| 122 La Casa Via, Ste. 223 |
| Walnut Creek, 925-943-6800 |
| Alta Bates Summit Medical Center–Alta Bates Campus |
| ORTHOPEDIC SURGERY |
| Lesley J. Anderson, MD |
| Knee injuries/ACL/meniscus tears, shoulder injuries, knee resurfacing, PRP (platelet rich plasma) |
| 2100 Webster St., Ste. 309 |
| San Francisco, 415-923-3029 |
| California Pacific Medical Center–Pacific Campus |
| David M. Bell, MD |
| Arthroscopic surgery, shoulder replacement, fractures–complex, rotator cuff surgery |
| 5924 Stoneridge Dr., Ste. 202 |
| Pleasanton, 925-600-7020 |
| ValleyCare Medical Center–Pleasanton |
| Sigurd H. Berven, MD |
| Spinal disorders, spinal surgery–pediatric & adult, spinal disorders–degenerative, spinal deformity |
| 400 Parnassus Ave., Floor 3 |
| San Francisco, 415-353-2739 |
| UCSF Medical Center |
| John T. Dearborn, MD |
| Arthritis-hip & knee, hip replacement & revision, knee replacement & revision |
| 2000 Mowry Ave. |
| Fremont, 510-818-7200 |
| Washington Hospital |
| Stuart B. Goodman, MD/PhD |
| Reconstructive surgery, hip replacement & revision, knee replacement & revision, osteonecrosis |
| 2450 Broadway St., Pavilion A–1st Floor |
| Redwood City, 650-723-5643 |
| Stanford University Hospital & Clinics |
| Kevin K. Howe, MD |
| Arthritis–hip & knee, hip replacement |
| 208 Concourse Blvd., Ste. 1 |
| Santa Rosa, 707-544-3400 |
| Santa Rosa Memorial Hospital |
| Ken Y. Hsu, MD |
| Spinal surgery, spinal disorders, pediatric orthopedic surgery |
| 1 Shrader St., Ste. 450 |
| San Francisco, 415-750-5570 |
| St. Mary’s Medical Center–San Francisco |
| John M. Knight, MD |
| Joint replacement, arthroscopic surgery–hip, joint reconstruction, sports injuries |
| 2405 Shadelands Dr. |
| Walnut Creek, 925-939-8585 |
| John Muir Medical Center |
| David W. Lowenberg, MD |
| Trauma, limb lengthening (Ilizarov procedure), fractures–complex & non-union, limb sparing surgery |
| 450 Broadway St. |
| Redwood City, 650-723-5643 |
| Stanford University Hospital & Clinics |
| Richard J. O’Donnell, MD |
| Bone cancer, sarcoma–soft tissue, pediatric orthopedic cancers |
| 1825 4th St., Floor 4 |
| San Francisco, 415-885-3800 |
| UCSF Medical Center |
| Nirav K. Pandya, MD |
| Pediatric orthopedic surgery, pediatric sports medicine, trauma–pediatric, sports injuries |
| 744 52nd St. |
| Oakland, 510-428-3238 |
| UCSF Benioff Children’s Hospital Oakland |
| Coleen S. Sabatini, MD |
| Pediatric orthopedic surgery, trauma, scoliosis, fractures |
| 744 52nd St. |
| Oakland, 510-428-3238 |
| UCSF Benioff Children’s Hospital Oakland |
| Michael W. Shifflett, MD |
| Sports medicine, arthroscopic surgery, joint replacement, trauma |
| 3273 Claremont Way, Ste. 100 |
| Napa, 707-254-7117 |
| Queen of the Valley Hospital |
| Paul J. Slosar, MD |
| Spinal surgery, minimally invasive spinal surgery, spinal reconstructive surgery, spinal surgery–cervical |
| 455 Hickey Blvd., Ste. 310 |
| Daly City, 650-985-7500 |
| Seton Medical Center–Daly City, CA |
| Robert Teasdale, MD |
| Sports injuries, reconstructive surgery |
| 1375 S. Eliseo Dr., Ste. D |
| Greenbrae, 415-461-4150 |
| Marin General Hospital |
| Louay Toma, MD |
| Sports medicine, trauma, minimally invasive surgery, hip replacement–anterior approach |
| 2405 Shadelands Dr. |
| Walnut Creek, 925-939-8585 |
| John Muir Medical Center |
| Thomas P. Vail, MD |
| Hip & knee replacement, hip resurfacing, arthritis, osteonecrosis |
| 1500 Owens St., Floor 4 |
| San Francisco, 415-353-2808 |
| UCSF Medical Center |
| James Zucherman, MD |
| Spinal surgery, spinal disorders–degenerative, pediatric orthopedic surgery |
| 1 Shrader St., Ste. 450 |
| San Francisco, 415-750-5570 |
| St. Mary’s Medical Center–San Francisco |
| OTOLARYNGOLOGY |
| Ivan H. El-Sayed, MD |
| Head & neck cancer, salivary gland tumors & surgery, sinus tumors, skull-base tumors |
| 1825 4th St., Ste. 4San Francisco, 415-885-7528 |
| UCSF Medical Center |
| Kevin M. Gersten, MD/PhD |
| Sleep disorders/apnea/snoring, sinus disorders/surgery, nasal & sinus disorders |
| 39650 Liberty St. |
| Fremont, 510-498-2689 |
| Washington Hospital |
| F. Christopher Holsinger, MD |
| Thyroid disorders, thyroid cancer & surgery, head & neck cancer, endoscopic surgery |
| 900 Blake Wilbur Dr., Floor 3 |
| Stanford, 650-498-6000 |
| Stanford University Hospital & Clinics |
| Mark R. Homicz, MD |
| Thyroid & parathyroid surgery, head & neck cancer, nasal & sinus surgery, reconstructive surgery |
| 1701 4th St., Ste. 120 |
| Santa Rosa, 707-523-7025 |
| Santa Rosa Memorial Hospital |
| Abraham G. Hsieh, MD |
| Sinus disorders/surgery, pediatric otolaryngology, sleep disorders/apnea/ snoring, head & neck cancer |
| 2623 Shadelands Dr. |
| Walnut Creek, 925-933-8462 |
| Stanford University Hospital & Clinics |
| Robert K. Jackler, MD |
| Neuro-otology, skull-base tumors, microsurgery, ear disorders |
| 2452 Watson Ct., Ste. 1700 |
| Palo Alto, 650-723-5281 |
| Stanford University Hospital & Clinics |
| Sam Most, MD |
| Facial plastic & reconstructive surgery, cosmetic surgery–face & neck, craniofacial surgery/reconstruction, facial paralysis |
| 801 Welch Rd. |
| Stanford, 650-736-3223 |
| Stanford University Hospital & Clinics |
| Lisa A. Orloff, MD |
| Thyroid & parathyroid cancer & surgery, microvascular surgery, head & neck cancer |
| 900 Blake Wilbur Dr., Floor 3 |
| Stanford, 650-498-6000 |
| Stanford University Hospital & Clinics |
| Timothy A. Scott, MD |
| Facial plastic surgery, head & neck surgery |
| 2623 Shadelands Dr. |
| Walnut Creek, 925-933-8462 |
| Stanford University Hospital & Clinics |
| Mark I. Singer, MD |
| Voice disorders, laryngeal disorders, reconstructive surgery, head & neck cancer |
| 2340 Clay St., Floor 2 |
| San Francisco, 415-600-3898 |
| California Pacific Medical Center–Pacific Campus |
| Chih-Kwang Sung, MD |
| Voice disorders, voice disorders/professional voice care, swallowing disorders, airway disorders |
| 801 Welch Rd. |
| Stanford, 650-723-5281 |
| Stanford University Hospital & Clinics |
| John Sunwoo, MD |
| Head & neck cancer, melanoma–head & neck, thyroid & parathyroid cancer & surgery |
| 875 Blake Wilbur Dr., Clinic B |
| Palo Alto, 650-498-6000 |
| Stanford University Hospital & Clinics |
| Winston C. Vaughan, MD |
| Endoscopic sinus surgery, sinus surgery–complex, nasal & sinus disorders |
| 3351 El Camino Real, Ste. 200 |
| Atherton, 650-399-4630 |
| Stanford University Hospital & Clinics |
| James C. Wu, MD |
| Facial plastic & reconstructive surgery, eyelid surgery/blepharoplasty, rhinoplasty, nasal & sinus surgery |
| 1800 Sullivan Ave., Ste. 411 |
| Daly City, 650-994-3223 |
| Seton Medical Center–Daly City, CA |
| Mark I. Zeme, MD |
| sinus disorders/surgery, thyroid & parathyroid surgery, pediatric otolaryngology |
| 20400 Lake Chabot Rd., Ste. 301, |
| Castro Valley, 510-889-6673 |
| Eden Medical Center |
| PAIN MEDICINE |
| Hoyman M. Hong, MD |
| Pain management, pain–musculoskeletal-spine & neck, pain-back & neck, pain–interventional techniques |
| 1199 Bush St., Ste. 300 |
| San Francisco, 415-353-6464 |
| St. Francis Memorial Hospital |
| Elliot J. Krane, MD |
| Pediatric pain medicine |
| 321 Middlefield Rd., Ste. 225 |
| Menlo Park, 650-497-8977 |
| Lucile Packard Children’s Hospital |
| Sean C. Mackey, MD/PhD |
| Pain–chronic, pain–cancer, pain–facial, pain–low back |
| 450 Broadway St., Pavilion A |
| Redwood City, 650-723-6238 |
| Stanford University Hospital & Clinics |
| PEDIATRIC CARDIOLOGY |
| Daniel Bernstein, MD |
| Transplant medicine–heart, congenital heart disease, heart failure |
| 725 Welch Rd., Ste. 181 |
| Palo Alto, 650-721-2121 |
| Lucile Packard Children’s Hospital |
| Michael M. Brook, MD |
| Echocardiography |
| 1825 4th St. |
| San Francisco, 415-353-2008 |
| UCSF Benioff Children’s Hospital San Francisco |
| Andrew J. Maxwell, MD |
| Fetal congenital and acquired heart disease, sports cardiology, dysautomonia, nutrition |
| 5933 Coronado Ln., Ste. 104 |
| Pleasanton, 925-416-0100 |
| Heart of the Valley Pediatric Cardiology |
| Howard M. Rosenfeld, MD |
| Congenital heart disease & acquired, fetal cardiology, cardiac catheterization, echocardiography |
| 747 52nd St. |
| Oakland, 510-428-3380 |
| UCSF Benioff Children’s Hospital Oakland |
| David N. Rosenthal, MD |
| Heart failure, transplant medicine–heart, cardiomyopathy |
| 725 Welch Rd., Ste. 181 |
| Palo Alto, 650-721-2121 |
| Lucile Packard Children’s Hospital |
| David F. Teitel, MD |
| Cardiac catheterization, congenital heart disease |
| 1825 4th St. |
| San Francisco, 415-353-2008 |
| UCSF Benioff Children’s Hospital San Francisco |
| PEDIATRIC ENDOCRINOLOGY |
| Tandy Aye, MD |
| Diabetes |
| 730 Welsh Rd. |
| Palo Alto, 650-736-7642 |
| Lucile Packard Children’s Hospital |
| Robert H. Lustig, MD |
| Obesity, metabolic syndrome, neuroendocrine disorders, hyperinsulinism |
| 550 16th St., Floor 4, MS 0434 |
| San Francisco, 415-476-7953 |
| UCSF Benioff Children’s Hospital San Francisco |
| Stephen M. Rosenthal, MD |
| Sexual development disorders, diabetes |
| 1825 4th St., Floor 6 |
| San Francisco, 415-353-7337 |
| UCSF Benioff Children’s Hospital San Francisco |
| PEDIATRIC GASTROENTEROLOGY |
| Adel B. Abi-Hanna, MD |
| 14777 Los Gatos Blvd., Ste. 200 |
| Los Gatos, 408-358-3573 |
| Lucile Packard Children’s Hospital |
| Sabina Ali, MD |
| 106 La Casa Via, Ste. 100 |
| Walnut Creek, 925-239-2900 |
| Lucile Packard Children’s Hospital |
| Elizabeth E. Gleghorn, MD |
| Pain–abdominal recurrent, feeding disorders, liver disease, hepatitis |
| 744 52nd St., Floor 5 |
| Oakland, 510-428-3058 |
| UCSF Benioff Children’s Hospital Oakland |
| Melvin B. Heyman, MD |
| Inflammatory bowel disease/Crohn’s, nutrition in bowel disorders |
| 1825 4th St., Floor 6 |
| San Francisco, 415-353-2813 |
| UCSF Benioff Children’s Hospital San Francisco |
| Sue J. Rhee, MD |
| Liver disease, transplant medicine–liver |
| 1825 4th St., Floor 6 |
| San Francisco, 415-353-2813 |
| UCSF Benioff Children’s Hospital San Francisco |
| PEDIATRIC HEMATOLOGY-ONCOLOGY |
| Anuradha Banerjee, MD |
| Brain tumors |
| 1825 4th St., Floor 6 |
| San Francisco, 415-476-3831 |
| UCSF Medical Center |
| James H. Feusner, MD |
| Leukemia, Wilms’ tumor, liver cancer |
| 747 52nd St. |
| Oakland, 510-428-3372 |
| UCSF Benioff Children’s Hospital Oakland |
| Michael P. Link, MD |
| Hodgkin’s lymphoma, lymphoma, non-Hodgkin’s, sarcoma |
| 725 Welch Rd. |
| Palo Alto, 650-497-8953 |
| Lucile Packard Children’s Hospital |
| Neyssa Marina, MD |
| Sarcoma, cancer survivors–late effects of therapy, sarcoma–soft tissue |
| 725 Welch Rd., #150 |
| Palo Alto, 650-497-8953 |
| Lucile Packard Children’s Hospital |
| Katherine K. Matthay, MD |
| Neuroblastoma, bone marrow transplant |
| 1825 4th St., Floor 6 |
| San Francisco, 415-476-3831 |
| UCSF Benioff Children’s Hospital San Francisco |
| Elliott P. Vichinsky, MD |
| Hematologic disorders, thalassemia, sickle cell disease |
| 747 52nd St. |
| Oakland, 510-428-3372 |
| UCSF Benioff Children’s Hospital Oakland |
| PEDIATRIC INFECTIOUS DISEASE |
| Francesca R. Geertsma, MD |
| 3700 California St., Ste. B555 |
| San Francisco, 415-600-0770 |
| California Pacific Medical Center–California Campus |
| Ann M. Petru, MD |
| HIV/AIDS |
| 744 52nd St. |
| Oakland, 510-428-3336 |
| UCSF Benioff Children’s Hospital Oakland |
| PEDIATRIC NEPHROLOGY |
| Steven R. Alexander, MD |
| Kidney failure, transplant medicine–kidney, nephrotic syndrome, dialysis care |
| 770 Welch Rd., Ste. 300 |
| Palo Alto, 650-724-0353 |
| Lucile Packard Children’s Hospital |
| Paul C. Grimm, MD |
| Transplant medicine–kidney, cystinosis |
| 770 Welch Rd., Ste. 300 |
| Palo Alto, 650-724-0353 |
| Lucile Packard Children’s Hospital |
| Elizabeth M. Talley, MD |
| Kidney disease–chronic, transplant medicine–kidney, dialysis care |
| 6121 Hollis St., Ste. 2 |
| Emeryville, 650-721-5807 |
| Lucile Packard Children’s Hospital |
| PEDIATRIC OTOLARYNGOLOGY |
| Kay W. Chang, MD |
| Cochlear implants, hearing loss, ear reconstruction/microtia, otology |
| 2452 Watson Ct., Floor 1 |
| Palo Alto, 650-724-4800 |
| Lucile Packard Children’s Hospital |
| Kristina W. Rosbe, MD |
| Airway disorders, neck masses, sinus disorders/surgery |
| 1825 4th St., Floor 5 |
| San Francisco, 415-353-2757 |
| UCSF Benioff Children’s Hospital San Francisco |
| Erin J. Simms-Edwards, MD |
| 2316 Dwight Way |
| Berkeley, 510-845-4500 |
| UCSF Benioff Children’s Hospital Oakland |
| PEDIATRIC PULMONOLOGY |
| David N. Cornfield, MD |
| Cystic fibrosis, critical care, respiratory failure |
| 770 Welch Rd., Ste. 380 |
| Palo Alto, 650-497-4478 |
| Lucile Packard Children’s Hospital |
| Karen Ann Hardy, MD |
| Cystic fibrosis, asthma & chronic lung disease, respiratory failure, ventilation management–long term |
| 6121 Hollis St., Ste. 2 |
| Emeryville, 844-724-4140 |
| California Pacific Medical Center–California Campus |
| Ngoc Phuong Ly, MD |
| Asthma, bronchopulmonary dysplasia, respiratory failure, cystic fibrosis |
| 1825 4th St., Floor 6 |
| San Francisco, 415-353-7337 |
| UCSF Benioff Children’s Hospital San Francisco |
| Dennis W. Nielson, MD/PhD |
| Cystic fibrosis, chronic lung disease of infancy |
| 1825 4th St., Floor 6 |
| San Francisco, 415-353-7337 |
| UCSF Benioff Children’s Hospital San Francisco |
| PEDIATRIC RHEUMATOLOGY |
| Tzielan C. Lee, MD |
| 730 Welch Rd., Floor 2 |
| Palo Alto, 650-723-8295 |
| Lucile Packard Children’s Hospital |
| Emily von Scheven, MD |
| Rheumatic diseases of childhood, lupus/SLE, juvenile arthritis |
| 1825 4th St., Floor 6 |
| San Francisco, 415-353-7337 |
| UCSF Benioff Children’s Hospital San Francisco |
| PEDIATRIC SURGERY |
| James M. Betts, MD |
| Trauma |
| 744 52nd St., Ste. 4100 |
| Oakland, 510-428-3022 |
| UCSF Benioff Children’s Hospital Oakland |
| Gary E. Hartman, MD |
| Laparoscopic surgery, thoracic surgery |
| 14601 S. Bascom Ave., Ste. 200 |
| Los Gatos, 408-879-9153 |
| Lucile Packard Children’s Hospital |
| Thomas Tin Leung Hui, MD |
| Gastrointestinal surgery, neonatal surgery–gastrointestinal, congenital anomalies–gastrointestinal |
| 744 52nd St., Ste. 4100 |
| Oakland, 510-428-3022 |
| UCSF Benioff Children’s Hospital Oakland |
| Olajire Idowu, MD |
| 744 52nd St., Ste. 4100 |
| Oakland, 510-428-3022 |
| UCSF Benioff Children’s Hospital Oakland |
| Hanmin Lee, MD |
| Fetal surgery, neonatal surgery, minimally invasive surgery, congenital anomalies |
| 1825 4th St., Floor 5 |
| San Francisco, 415-476-2538 |
| UCSF Benioff Children’s Hospital San Francisco |
| Karl G. Sylvester, MD |
| Fetal surgery, trauma, vascular malformations |
| 730 Welch Rd., Floor 2 |
| Palo Alto, 650-723-4800 |
| Lucile Packard Children’s Hospital |
| PEDIATRIC UROLOGY |
| Laurence S. Baskin, MD |
| Genitourinary reconstruction, varicocele in adolescents, hypospadias, fetal urology |
| 1825 4th St., Floor 5 |
| San Francisco, 415-353-2200 |
| UCSF Benioff Children’s Hospital San Francisco |
| William A. Kennedy, MD |
| 750 Welch Rd., Ste. 218 |
| Palo Alto, 650-723-9779 |
| Lucile Packard Children’s Hospital |
| PHYSICAL MEDICINE & REHABILITATION |
| Christine M. Aguilar, MD |
| Pediatric rehabilitation, spina bifida, spasticity management, neurologic rehabilitation |
| 747 52nd St., Ste. 203 |
| Oakland, 510-428-3655 |
| UCSF Benioff Children’s Hospital Oakland |
| Yung Chuan Chen, MD |
| Spinal rehabilitation, sports medicine, pain management, musculoskeletal disorders |
| 101 S. San Mateo Dr., Ste. 301 |
| San Mateo, 650-558-1802 |
| Sequoia Hospital |
| Jeff Shou-Ping Chen, MD |
| Integrative medicine, pain management |
| 450 N. Wiget Ln. |
| Walnut Creek, 925-691-9806 |
| John Muir Medical Center |
| Elaine Date, MD |
| Spinal rehabilitation, electrodiagnosis, Botox therapy, acupuncture |
| 363 Main St., Ste. C |
| Redwood City, 650-306-9490 |
| Mills–Peninsula Medical Center |
| Carl W. Fieser, MD |
| Pain–interventional techniques, sports medicine, electrodiagnosis, pain management |
| 450 N. Wiget Ln. |
| Walnut Creek, 925-691-9806 |
| Sutter Delta Medical Center |
| Robert R. Haining, MD |
| Pediatric rehabilitation, spina bifida, cerebral palsy, brain injury rehabilitation–pediatric |
| 747 52nd St., Ste. 203 |
| Oakland, 510-428-3655 |
| UCSF Benioff Children’s Hospital Oakland |
| Corby S. Kessler, MD |
| Integrative medicine |
| 935 Trancas St., Ste. 1B |
| Napa, 707-255-6115 |
| Queen of the Valley Hospital |
| Stephen Ng, MD |
| Spasticity management, spinal cord injury rehabilitation, stroke rehabilitation |
| 45 Castro St., Ste. 200 |
| San Francisco, 415-600-7710 |
| California Pacific Medical Center–Davies Campus |
| Scott A. Rome, MD |
| Brain injury rehabilitation, stroke rehabilitation, electrodiagnosis, spasticity management |
| 45 Castro St., Ste. 200 |
| San Francisco, 415-600-7710 |
| California Pacific Medical Center–Davies Campus |
| Jeffrey A. Saal, MD |
| Pain–lower back (IDET procedure), spinal rehabilitation, sports medicine, musculoskeletal disorders |
| 500 Arguello St., Ste. 100 |
| Redwood City, 650-995-1207 |
| Ernest A. Sponzilli, MD |
| Pain management, spinal rehabilitation, pain–interventional techniques, pain-spine |
| 2 Bon Air Rd., Ste. 120 |
| Larkspur, 415-927-5300 |
| Marin General Hospital |
| PLASTIC SURGERY |
| Carolyn C. Chang, MD |
| Cosmetic surgery–face & body, cosmetic surgery–breast, facial rejuvenation |
| 2100 Webster St., Ste. 508 |
| San Francisco, 415-923-3070 |
| California Pacific Medical Center–Pacific Campus |
| Stephen P. Daane, MD |
| Pediatric plastic surgery, reconstructive plastic surgery, gynecomastia, ear reshaping (otoplasty) |
| 2186 Geary Blvd., Ste. 212 |
| San Francisco, 415-561-0542 |
| California Pacific Medical Center–Pacific Campus |
| Tancredi F. D’Amore, MD |
| Cosmetic surgery–face & body, cosmetic surgery–breast, breast reconstruction, liposuction & body contouring |
| 21 Tamal Vista Blvd., Ste. 103 |
| Corte Madera, 415-927-7660 |
| Marin General Hospital |
| Miguel A. Delgado, MD |
| Cosmetic surgery–face, cosmetic surgery–breast, cosmetic surgery–body, gynecomastia |
| 165 Rowland Way, Ste. 300 |
| Novato, 415-898-4161 |
| Novato Community Hospital |
| Michael C. Glafkides, MD |
| Cosmetic surgery–breast, liposuction & body contouring, eyelid surgery, cosmetic surgery–face |
| 101 S. San Mateo Dr., Ste. 200 |
| San Mateo, 650-347-7900 |
| Mills–Peninsula Medical Center |
| Geoffrey C. Gurtner, MD |
| Microsurgery, breast reconstruction, wound healing/care |
| 900 Blake Wilbur Dr. |
| Stanford, 650-498-6004 |
| Stanford University Hospital & Clinics |
| William Y. Hoffman, MD |
| Pediatric plastic surgery, cleft palate/lip, craniofacial surgery, reconstructive microvascular surgery |
| 350 Parnassus Ave., Ste. 509 |
| San Francisco, 415-353-4201 |
| UCSF Medical Center |
| Karen M. Horton, MD |
| Cosmetic surgery–breast, cosmetic surgery–body, liposuction & body contouring, breast reconstruction |
| 2100 Webster St., Ste. 506 |
| San Francisco, 415-923-3067 |
| California Pacific Medical Center–Davies Campus |
| Rebecca L. Jackson, MD |
| Cosmetic surgery, microvascular surgery, tattoo removal |
| 1175 Trancas St. |
| Napa, 707-258-6053 |
| Queen of the Valley Hospital |
| Yvonne L. Karanas, MD |
| Burns–reconstructive plastic surgery |
| 751 S. Bascom Ave. |
| San Jose, 888-334-1000 |
| Santa Clara Valley Medical Center |
| Timothy J. Marten, MD |
| Cosmetic surgery–face & neck, racial rejuvenation |
| 450 Sutter St., Ste. 2222 |
| San Francisco, 415-677-9937 |
| California Pacific Medical Center–Pacific Campus |
| Frank J. Piro, MD |
| Cosmetic surgery–face, eyelid surgery, breast augmentation, liposuction & body contouring |
| 50 S San Mateo Dr., Ste. 470 |
| San Mateo, 650-652-8230 |
| Mills–Peninsula Medical Center |
| James J. Romano, MD |
| Liposuction & body contouring, cosmetic surgery–breast, facial rejuvenation, tuberous breasts |
| 1650 Jackson St., Ste. 101 |
| San Francisco, 415-981-3911 |
| California Pacific Medical Center–California Campus |
| Jane S. Weston, MD |
| Cosmetic surgery–face, cosmetic surgery–breast, liposuction & body contouring, facial rejuvenation |
| 3351 El Camino Real, Ste. 201 |
| Atherton, 650-363-0300 |
| Stanford University Hospital & Clinics |
| PSYCHIATRY |
| Daniel F. Becker, MD |
| Addiction psychiatry, adolescent psychiatry, behavioral disorders, psychodynamic psychotherapy |
| 345 Lorton Av.e, Ste. 104 |
| Burlingame, 650-696-5912 |
| Mills–Peninsula Medical Center |
| Terence A. Ketter, MD |
| Bipolar/mood disorders, psychopharmacology |
| 401 Quarry Rd. |
| Stanford, 650-723-8335 |
| Stanford University Hospital & Clinics |
| Elizabeth J. Mahler, MD |
| Liaison psychiatry, crisis intervention, behavioral disorders, anxiety & depression |
| 3130 Alpine Rd., Ste. 180 |
| Portola Valley, 650-327-0808 |
| Stanford University Hospital & Clinics |
| Victor I. Reus, MD |
| Psychopharmacology, bipolar/mood disorders, behavioral disorders, depression |
| 401 Parnassus Ave. |
| San Francisco, 415-476-7478 |
| Langley Porter Psychiatric Hospital & Clinics |
| David Spiegel, MD |
| Psychiatry in cancer, hypnosis, post traumatic stress disorder, psychotherapy |
| 401 Quarry Rd., Floor 2 |
| Stanford, 650-498-9111 |
| Stanford University Hospital & Clinics |
| PULMONARY DISEASE |
| Jason S. Chu, MD |
| Pulmonary rehabilitation |
| 2557 Mowry Ave., Ste. 12 |
| Fremont, 510-248-1550 |
| Washington Hospital |
| Ryan H. Dougherty, MD |
| Asthma, cystic fibrosis, interstitial lung disease, sarcoidosis |
| 2351 Clay St., Ste. 501 |
| San Francisco, 415-923-3421 |
| California Pacific Medical Center–California Campus |
| Robert M. Jasmer, MD |
| Critical care |
| 1720 El Camino Real, Ste. 150 |
| Burlingame, 650-697-5367 |
| Mills–Peninsula Medical Center |
| Gary M. LeKander, MD |
| Asthma, chronic obstructive lung disease (COPD), occupational lung disease, lung cancer |
| 1312 Prentice Dr. |
| Healdsburg, 707-431-6314 |
| Healdsburg District Hospital |
| Merrill R. Nisam, MD |
| Asthma, pneumonia, chronic obstructive lung disease (COPD), pulmonary hypertension |
| 1260 S. Eliseo Dr., Floor 2 |
| Greenbrae, 415-924-1214 |
| Marin General Hospital |
| Norman W. Rizk, MD |
| Chronic obstructive lung disease (COPD), interstitial lung disease |
| 300 Pasteur Dr., Floor 1 |
| Stanford, 650-725-7061 |
| Stanford University Hospital & Clinics |
| Helena L. Wang, MD |
| Pulmonary hypertension, chronic obstructive lung disease (COPD), sarcoidosis |
| 2351 Clay St., Ste. 501 |
| San Francisco, 415-923-3421 |
| California Pacific Medical Center–California Campus |
| Roham T. Zamanian, MD |
| Pulmonary hypertension, pulmonary embolism |
| 300 Pasteur Dr., Floor 1 |
| Stanford, 650-725-7061 |
| Stanford University Hospital & Clinics |
| RADIATION ONCOLOGY |
| Lisa K. Boohar, MD |
| Brachytherapy, intensity modulated radiotherapy (IMRT), breast cancer, palliative care |
| 170 Alameda de Las Pulgas |
| Redwood City, 650-367-5591 |
| Sequoia Hospital |
| Mark K. Buyyounouski, MD |
| Genitourinary cancer, prostate cancer, brachytherapy, stereotactic radiosurgery |
| 875 Blake Wilbur Dr., Clinic D |
| Stanford, 650-723-6171 |
| Stanford University Hospital & Clinics |
| Nam K. Cho, DO/PhD |
| 751 S. Bascom Ave. |
| San Jose, 888-334-1000 |
| Santa Clara Valley Medical Center |
| Maximilian Diehn, MD |
| Lung cancer, esophageal cancer, thymoma and thymic cancer |
| 875 Blake Wilbur Dr., Clinic D |
| Stanford, 650-498-6339 |
| Stanford University Hospital & Clinics |
| Francine Halberg, MD |
| Breast cancer |
| 1350 S. Eliseo Dr., Ste. 100 |
| Greenbrae, 415-925-7326 |
| Marin General Hospital |
| Steven Hancock, MD |
| Genitourinary cancer, prostate cancer, central nervous system cancer, clinical trials |
| 875 Blake Wilbur Dr., Clinic D |
| Stanford, 650-723-6171 |
| Stanford University Hospital & Clinics |
| Wendy Y. Hara, MD |
| Head & neck cancer, skin cancer, stereotactic body radiotherapy |
| 875 Blake Wilbur Dr., Clinic D |
| Stanford, 650-736-0845 |
| Stanford University Hospital & Clinics |
| Kathleen C. Horst, MD |
| Breast cancer |
| 875 Blake Wilbur Dr., Clinic D |
| Stanford, 650-736-0845 |
| Stanford University Hospital & Clinics |
| Albert C. Koong, MD/PhD |
| Gastrointestinal cancer, pancreatic cancer, liver cancer |
| 875 Blake Wilbur Dr., Clinic D |
| Stanford, 650-723-6171 |
| Stanford University Hospital & Clinics |
| David A. Larson, MD/PhD |
| Neuro-oncology, brain tumors, stereotactic radiosurgery |
| 2500 Mowry Ave., Ste. 222 |
| Fremont, 510-818-1160 |
| Washington Hospital |
| Quynh-Thu Xuan Le, MD |
| Head & neck cancer, lung cancer, thoracic cancers, clinical trials |
| 875 Blake Wilbur Dr., Clinic D |
| Stanford, 650-736-0845 |
| Stanford University Hospital & Clinics |
| Billy W. Loo, MD/PhD |
| Lung cancer, thoracic cancers, stereotactic radiosurgery |
| 875 Blake Wilbur Dr. |
| Palo Alto, 650-498-6000 |
| Stanford University Hospital & Clinics |
| John L. Meyer, MD |
| Intensity modulated radiotherapy (IMRT) |
| 900 Hyde St., Level B |
| San Francisco, 415-353-6420 |
| St. Francis Memorial Hospital |
| Catherine C. Park, MD |
| Breast cancer |
| 1600 Divisadero St., Ste. H1031 |
| San Francisco, 415-353-7175 |
| UCSF Medical Center |
| James L. Rembert, MD |
| Stereotactic radiosurgery, gastrointestinal cancer, head & neck cancer, brain tumors |
| 2001 Dwight Way |
| Berkeley, 510-204-5311 |
| Alta Bates Summit Medical Center–Alta Bates Campus |
| Scott G. Soltys, MD |
| Brain tumors, spinal tumors |
| 875 Blake Wilbur Dr., Clinic D |
| Stanford, 650-736-0845 |
| Stanford University Hospital & Clinics |
| REPRODUCTIVE ENDOCRINOLOGY |
| Valerie L. Baker, MD |
| Ovarian failure, infertility |
| 1195 W. Fremont Ave., Ste. 1 |
| Sunnyvale, 650-498-7911 |
| Stanford University Hospital & Clinics |
| Marcelle I. Cedars, MD |
| Infertility-IVF, polycystic ovarian syndrome, menopause problems |
| 499 Illinois St., Floor 6 |
| San Francisco, 415-353-7475 |
| UCSF–Mount Zion Medical Center |
| Philip E. Chenette, MD |
| Infertility–IVF, fertility preservation, infertility–advanced maternal age |
| 55 Francisco St., Ste. 500 |
| San Francisco, 415-834-3000 |
| California Pacific Medical Center–California Campus |
| Linda C. Giudice, MD/PhD |
| Infertility–IVF, endometriosis |
| 499 Illinois St., Floor 6 |
| San Francisco, 415-353-7475 |
| UCSF Medical Center |
| Carolyn R. Givens, MD |
| Prenatal genetic diagnosis, Infertility-IVF, laparoscopic surgery, hysteroscopic surgery |
| 55 Francisco St., Floor 5 |
| San Francisco, 415-834-3000 |
| California Pacific Medical Center–Pacific Campus |
| Carl M. Herbert, MD |
| Infertility–IVF |
| 55 Francisco St., Ste. 500 |
| San Francisco, 415-834-3000 |
| California Pacific Medical Center–California Campus |
| Isabelle P. Ryan, MD |
| Infertility–IVF, endometriosis, fertility preservation |
| 55 Francisco St., Ste. 500 |
| San Francisco, 415-834-3000 |
| California Pacific Medical Center–Pacific Campus |
| Eldon D. Schriock, MD |
| Infertility–IVF |
| 55 Francisco St., Ste. 500 |
| San Francisco, 415-834-3000 |
| California Pacific Medical Center–California Campus |
| Collin B. Smikle, MD |
| Infertility–IVF, laparoscopic surgery, polycystic ovarian syndrome |
| 1700 California St., Ste. 570 |
| San Francisco, 415-673-9199 |
| California Pacific Medical Center–California Campus |
| Peter Uzelac, MD |
| Infertility–IVF, fertility preservation, complementary medicine |
| 1100 S. Eliseo Dr., Ste. 107 |
| Greenbrae, 415-925-9404 |
| Marin General Hospital |
| Susan P. Willman, MD |
| Infertility–IVF, preimplantation genetic diagnosis, laparoscopic surgery, robotic surgery |
| 89 Davis Rd., Ste. 280 |
| Orinda, 925-867-1800 |
| John Muir Medical Center |
| RHEUMATOLOGY |
| Neal S. Birnbaum, MD |
| Arthritis, scleroderma |
| 2100 Webster St., Ste. 112 |
| San Francisco, 415-923-3060 |
| California Pacific Medical Center–Pacific Campus |
| Brian R. Kaye, MD |
| Rheumatoid arthritis, gout |
| 2999 Regent St., Ste. 301 |
| Berkeley, 510-204-8120 |
| Alta Bates Summit Medical Center–Alta Bates Campus |
| R. Elaine Lambert, MD |
| Musculoskeletal disorders, osteoarthritis |
| 500 Arguello St., Ste. 100 |
| Redwood City, 650-995-1204 |
| Stanford University Hospital & Clinics |
| Molly D. Magnano, MD |
| Arthritis |
| 2999 Regent St., Ste. 301 |
| Berkeley, 510-204-8120 |
| Alta Bates Summit Medical Center–Alta Bates Campus |
| SLEEP MEDICINE |
| Christopher R. Brown, MD |
| Sleep & snoring disorders, sleep disorders/apnea |
| 2351 Clay St., Ste. 501 |
| San Francisco, 415-923-3421 |
| California Pacific Medical Center–California Campus |
| Melissa S. Lim, MD |
| Sleep disorders/apnea, narcolepsy |
| 170 Alameda de Las Pulgas |
| Redwood City, 415-925-1416 |
| Sequoia Hospital |
| Brandon S. Lu, MD |
| Sleep & snoring disorders, sleep disorders/apnea |
| 2351 Clay St., Ste. 501 |
| San Francisco, 415-923-3421 |
| California Pacific Medical Center–California Campus |
| SPORTS MEDICINE |
| Ty P. Affleck, MD |
| Sports injuries, concussion, primary care sports medicine |
| 1255 N. Dutton Ave. |
| Santa Rosa, 707-546-9400 |
| Sutter Santa Rosa Regional Hospital |
| Christina R. Allen, MD |
| Knee injuries/ACL/meniscus tears, shoulder injuries, sports medicine–women |
| 1500 Owens St. |
| San Francisco, 415-353-2808 |
| UCSF Medical Center |
| Kambiz Behzadi, MD |
| Knee injuries/ACL, rotator cuff surgery, knee replacement, robotic surgery |
| 4626 Willow Rd. |
| Pleasanton, 925-463-0470 |
| ValleyCare Medical Center–Pleasanton |
| Ashay Kale, MD |
| Reconstructive surgery, shoulder & elbow surgery, arthroscopic surgery, rotator cuff surgery |
| 39350 Civic Center Dr., Ste. 300 |
| Fremont, 510-797-3933 |
| Washington Hospital |
| Anthony C. Luke, MD |
| Primary care sports medicine, sports injuries, running injuries |
| 1500 Owens St. |
| San Francisco, 415-353-2808 |
| UCSF Medical Center |
| C. Benjamin Ma, MD |
| Shoulder replacement, knee injuries/ACL/meniscus tears, arthroscopic surgery, elbow surgery |
| 1500 Owens St. |
| San Francisco, 415-353-2808 |
| UCSF Medical Center |
| Timothy R. McAdams, MD |
| Sports injuries, knee injuries, shoulder & elbow surgery, hand surgery |
| 450 Broadway St. |
| Redwood City, 800-717-0012 |
| UCSF Medical Center |
| Chad A. Roghair, MD |
| Musculoskeletal injuries, concussion |
| 25 Orinda Way, Ste. 100 |
| Orinda, 510-704-7760 |
| Alta Bates Summit Medical Center–Alta Bates Campus |
| Carlin H. Senter, MD |
| Primary care sports medicine, concussion, fractures–stress |
| 1500 Owens St. |
| San Francisco, 415-353-2808 |
| UCSF Medical Center |
| Daniel J. Solomon, MD |
| Shoulder surgery, rotator cuff surgery, reconstructive surgery, knee injuries/ACL/meniscus tears |
| 7100 Redwood Blvd., Ste. 200 |
| Novato, 415-492-1600 |
| Novato Community Hospital |
| SURGERY |
| Nancy L. Ascher, MD/PhD |
| Transplant–liver, transplant–kidney |
| 400 Parnassus Ave., Floor 7 |
| San Francisco, 415-353-1888 |
| UCSF Medical Center |
| William H. Brown, MD |
| hernia, hernia–sports |
| 556 Mowry Ave., Ste. 100 |
| Fremont, 510-793-2404 |
| Washington Hospital |
| Edward K. Chough, MD |
| Minimally invasive surgery |
| 3443 Villa Ln., Ste. 5 |
| Napa, 707-226-2031 |
| Queen of the Valley Hospital |
| Elizabeth A. Cunningham, MD |
| Breast cancer, melanoma, cancer surgery |
| 4 Financial Plaza |
| Napa, 707-266-7051 |
| Queen of the Valley Hospital |
| Quan-Yang Duh, MD |
| Endocrine surgery, thyroid & parathyroid cancer & surgery, adrenal tumors, minimally invasive surgery |
| 1600 Divisadero St., Floor 4 |
| San Francisco, 415-353-7687 |
| UCSF–Mount Zion Medical Center |
| Carlos O. Esquivel, MD/PhD |
| Transplant–liver (adult & pediatric), transplant–pancreas |
| 300 Pasteur Dr. |
| Stanford, 650-498-5689 |
| Stanford University Hospital & Clinics |
| Laura J. Esserman, MD |
| Breast cancer, breast surgery |
| 1600 Divisadero St., Floor 2 |
| San Francisco, 415-353-7070 |
| UCSF–Mount Zion Medical Center |
| Jessica E. Gosnell, MD |
| Thyroid & parathyroid surgery, thyroid cancer, endocrine surgery |
| 1600 Divisadero St., Floor 4 |
| San Francisco, 415-353-7687 |
| UCSF–Mount Zion Medical Center |
| Nima A. Grissom, MD |
| Breast cancer, breast surgery |
| 3801 Sacramento St., Ste. 100 |
| San Francisco, 415-600-1817 |
| California Pacific Medical Center–California Campus |
| Mary T. Hawn, MD |
| Gastrointestinal surgery, hernia, laparoscopic surgery, gastroesophageal reflux disease (GERD) |
| 900 Blake Wilbur Dr. |
| Stanford, 650-736-5800 |
| Stanford University Hospital & Clinics |
| Thomas Hirai, MD |
| Obesity/bariatric surgery, laparoscopic surgery, endoscopy, minimally invasive surgery |
| 200 Jose Figueres Ave., Ste. 225 |
| San Jose, 408-929-5610 |
| Regional Medical Center–San Jose |
| Gregg Jossart, MD |
| Obesity/bariatric surgery, gastrointestinal surgery, endocrine surgery |
| 2340 Clay St., Floor 2 |
| San Francisco, 415-923-3200 |
| California Pacific Medical Center–Pacific Campus |
| Mark Koransky, MD |
| Laparoscopic surgery, cancer surgery, gastrointestinal surgery |
| 3200 Kearney St., Floor 2 |
| Fremont, 510-498-2886 |
| Washington Hospital |
| Crystine M. Lee, MD |
| Gastrointestinal surgery, laparoscopic surgery |
| 5 Bon Air Rd., Ste. 101 |
| Larkspur, 415-924-2515 |
| Novato Community Hospital |
| Jonathan M. Levin, MD |
| Laparoscopic surgery |
| 165 Rowland Way, Ste. 312 |
| Novato, 415-898-6190 |
| Novato Community Hospital |
| John M. Morton, MD |
| Obesity/bariatric surgery minimally invasive surgery, natural orifice surgery (NOTES) |
| 900 Blake Wilbur Dr. |
| Palo Alto, 650-736-5800 |
| Stanford University Hospital & Clinics |
| Eric Nakakura, MD/PhD |
| Pancreatic cancer, liver cancer, gastrointestinal cancer, sarcoma–soft tissue |
| 1825 4th St., Floor 4 |
| San Francisco, 415-502-5577 |
| UCSF Medical Center |
| George Poultsides, MD |
| Gastrointestinal cancer, liver cancer, pancreatic cancer |
| 875 Blake Wilburm Dr., Clinic B |
| Stanford, 650-498-6000 |
| Stanford University Hospital & Clinics |
| John P. Roberts, MD |
| Transplant–liver, transplant–kidney |
| 505 Parnassus Ave., Ste. M896 |
| San Francisco, 415-353-1888 |
| UCSF Medical Center |
| Stanley J. Rogers, MD |
| Minimally invasive surgery, gastrointestinal surgery, obesity/bariatric surgery |
| 400 Parnassus Ave., Floor 6 |
| San Francisco, 415-353-2161 |
| UCSF Medical Center |
| Tobin M. Schneider, MD |
| Obesity/bariatric surgery, laparoscopic surgery, colon & rectal surgery, gastrointestinal surgery |
| 1101 S. San Mateo Dr., Ste. 104 |
| San Mateo, 650-342-1414 |
| Sequoia Hospital |
| THORACIC & CARDIAC SURGERY |
| Luis J. Castro, MD |
| Cardiovascular surgery, heart valve surgery–mitral, aortic surgery |
| 2900 Whipple Ave., Ste. 140 |
| Redwood City, 650-261-2366 |
| Sequoia Hospital |
| Murali Dharan, MD |
| Cardiac surgery–adult, heart valve surgery, minimally invasive cardiac surgery, minimally invasive thoracic surgery |
| 1320 El Capitan Dr., Ste. 120 |
| Danville, 925-676-2600 |
| John Muir Medical Center |
| Frank L. Hanley, MD |
| Pediatric cardiothoracic surgery, congenital heart disease–adult |
| 725 Welch Rd., Ste. 120 |
| Palo Alto, 650-724-2925 |
| Lucile Packard Children’s Hospital |
| Adam L. Harmon, MD |
| Cardiac surgery–adult, thoracic surgery |
| 2900 Whipple Ave., Ste. 140 |
| Redwood City, 650-261-2366 |
| Sequoia Hospital |
| Arthur C. Hill, MD |
| Cardiac surgery, thoracic surgery, trauma |
| 400 Parnassus Ave., Floor 6 |
| San Francisco, 415-353-1606 |
| UCSF Medical Center |
| James S. Hood, MD |
| Lung cancer, thoracic cancers, mediastinal tumors, cancer survivors–late effects of therapy |
| 2200 O’Farrell St., Floor 2 |
| San Francisco, 415-833-3800 |
| Kaiser Permanente South San Francisco Medical Center |
| David M. Jablons, MD |
| Lung cancer, mesothelioma, esophageal surgery |
| 1600 Divisadero St., Floor 4 |
| San Francisco, 415-885-3882 |
| UCSF–Mount Zion Medical Center |
| Keith F. Korver, MD |
| Coronary artery surgery, heart valve surgery, aneurysm–thoracic aortic, congenital heart disease |
| 3536 Mendocino Ave., Ste. 200 |
| Santa Rosa, 707-569-7860 |
| Sutter Santa Rosa Regional Hospital |
| Scot H. Merrick, MD |
| Heart valve surgery–mitral, minimally invasive cardiac surgery, congenital heart disease, arrhythmias |
| 400 Parnassus Ave., Floor 5 |
| San Francisco, 415-353-1606 |
| UCSF Medical Center |
| Olaf Reinhartz, MD |
| Pediatric cardiothoracic surgery, transplant–heart (pediatric) |
| 300 Pasteur Dr. |
| Stanford, 650-724-2925 |
| Lucile Packard Children’s Hospital |
| Joseph B. Shrager, MD |
| Lung cancer, thymoma and thymic cancer, emphysema–lung volume reduction, mediastinal tumors |
| 900 Blake Wilbur Dr. |
| Stanford, 650-498-6000 |
| Stanford University Hospital & Clinics |
| Russell D. Stanten, MD |
| Cardiothoracic surgery, minimally invasive heart valve Surgery, coronary artery surgery, esophageal surgery |
| 3300 Webster St., Ste. 500 |
| Oakland, 510-465-6600 |
| Alta Bates Summit Medical Center–Summit Campus |
| Y. Joseph Woo, MD |
| Minimally invasive cardiac surgery, robotic cardiac surgery, heart valve surgery–aortic, heart valve surgery–mitral |
| 300 Pasteur Dr., Ste. A31 |
| Stanford, 650-724-7500 |
| Stanford University Hospital & Clinics |
| UROGYNECOLOGY/FEMALE PELVIC MEDICINE & RECONSTRUCTIVE SURGERY |
| Alexandra L. Haessler, MD |
| Urogynecology, pelvic floor reconstruction, robotic surgery, laparoscopic surgery |
| 3838 California St., Ste. 305 |
| San Francisco, 415-367-9500 |
| California Pacific Medical Center–California Campus |
| Abner P. Korn, MD |
| Incontinence–urinary, pelvic organ prolapse repair, vaginal surgery, urogynecology |
| 2356 Sutter St., Floor 5 |
| San Francisco, 415-885-7788 |
| UCSF–Mount Zion Medical Center |
| Savitha Krishnan, MD |
| Urogynecology, pelvic reconstruction, pelvic organ prolapse repair, laparoscopic surgery |
| 2490 Hospital Dr., Ste. 111 |
| Mountain View, 650-934-7530 |
| El Camino Hospital |
| Heidi Wittenberg, MD |
| Urogynecology, laparoscopic surgery, pelvic organ prolapse repair, robotic surgery |
| 55 Francisco St., Ste. 300 |
| San Francisco, 415-395-9895 |
| California Pacific Medical Center–Pacific Campus |
| UROLOGY |
| Judson M. Brandeis, MD |
| Prostate cancer, minimally invasive surgery, kidney stones, vasectomy–no scalpel |
| 100 N. Wiget Ln., Ste. 290 |
| Walnut Creek, 925-937-7740 |
| John Muir Medical Center |
| Peter Bretan, MD |
| Transplant–kidney, laparoscopic kidney surgery, incontinence, urologic cancer |
| 1615 Hill Rd., Ste. 11 |
| Novato, 415-892-0904 |
| Novato Community Hospital |
| Peter R. Carroll, MD |
| Urologic cancer, urinary reconstruction, prostate cancer |
| 1825 4th St., Floor 4 |
| San Francisco, 415-353-7171 |
| UCSF Medical Center |
| Benjamin I. Chung, MD |
| Prostate cancer, kidney cancer, robotic surgery, prostate cancer/robotic surgery |
| 875 Blake Wilbur Dr., Clinic E |
| Stanford, 650-725-5544 |
| Stanford University Hospital & Clinics |
| Maxwell V. Meng, MD |
| Genitourinary cancer, laparoscopic surgery, robotic surgery |
| 1825 4th St., Floor 4 |
| San Francisco, 415-353-7171 |
| UCSF Medical Center |
| Joseph C. Presti, MD |
| Prostate cancer, bladder cancer, kidney cancer, testicular cancer |
| 3600 Broadway, Floor 4 |
| Oakland, 510-752-6796 |
| Kaiser Permanente Oakland Medical Center |
| Andrew G. Rosenberg, MD |
| Urologic cancer |
| 1750 El Camino Real, Ste. 307 |
| Burlingame, 650-259-1480 |
| Mills–Peninsula Medical Center |
| David M. Rudnick, MD |
| Minimally invasive surgery, kidney stones, incontinence, prostate benign disease |
| 1496 Professional Dr., Ste. 603 |
| Petaluma, 707-762-0059 |
| Novato Community Hospital |
| Parminder Sethi, MD |
| Neuro-urology, bladder reconstruction, incontinence, minimally invasive surgery |
| 100 N. Wiget Ln., Ste. 290 |
| Walnut Creek, 925-937-7740 |
| John Muir Medical Center |
| Eila C. Skinner, MD |
| Bladder cancer, bladder reconstruction, continent urinary diversions, urologic cancer |
| 875 Blake Wilbur Dr., Clinic E |
| Stanford, 650-725-5544 |
| Stanford University Hospital & Clinics |
| Marshall L. Stoller, MD |
| Kidney stones, minimally invasive surgery |
| 400 Parnassus Ave., Floor 6 |
| San Francisco, 415-353-2200 |
| UCSF Medical Center |
| C. Charles Wen, MD |
| Erectile dysfunction, kidney stones, kidney cancer, prostate cancer |
| 1320 El Capitan Dr., Ste. 320 |
| Danville, 925-866-2100 |
| Alta Bates Summit Medical Center–Summit Campus |
| VASCULAR & INTERVENTIONAL RADIOLOGY |
| David M. Hovsepian, MD |
| Uterine fibroid embolization, vascular malformations |
| 875 Blake Wilbur Dr. |
| Palo Alto, 650-724-7362 |
| Stanford University Hospital & Clinics |
| Robert Keith Kerlan, MD |
| Liver cancer, portal hypertension |
| 505 Parnassus Ave. |
| San Francisco, 415-353-1300 |
| UCSF Medical Center |
| Ralph Koenker, MD |
| Interventional radiology, neuroradiology, vascular disease |
| 504 Redwood Blvd., Ste. 300 |
| Novato, 415-925-7080 |
| Novato Community Hospital |
| Jeanne M. LaBerge, MD |
| Interventional radiology, uterine fibroid embolization |
| 505 Parnassus Ave. |
| San Francisco, 415-353-1300 |
| UCSF–Mount Zion Medical Center |
| Myron Marx, MD |
| Interventional radiology |
| 2333 Buchanan St., Floor 2 |
| San Francisco, 415-600-3232 |
| California Pacific Medical Center–Pacific Campus |
| VASCULAR SURGERY |
| Melinda Luz Aquino, MD |
| Endovascular surgery, minimally invasive surgery, vein disorders, varicose veins |
| 1850 Sullivan Ave., Ste. 300 |
| Daly City, 650-991-1122 |
| Seton Medical Center–Daly City, CA |
| Dirk S. Baumann, MD |
| Endovascular surgery, dialysis access, aneurysm–abdominal aortic, carotid endarterectomy |
| 1501B Trousdale Dr., Floor 5 |
| Burlingame, 650-652-8787 |
| Mills–Peninsula Medical Center |
| Michael S. Conte, MD |
| Aortic surgery, aneurysm, carotid endarterectomy, peripheral vascular disease |
| 400 Parnassus Ave., Ste. 501 |
| San Francisco, 415-353-2357 |
| UCSF Medical Center |
| Ronald L. Dalman, MD |
| Aortic surgery, peripheral vascular disease, limb salvage |
| 300 Pasteur Dr., Floor 3 |
| Stanford, 650-725-5227 |
| Stanford University Hospital & Clinics |
| Raju H. Gandhi, MD |
| 1850 El Camino Real, Ste. 200 |
| Burlingame, 650-697-2431 |
| Mills–Peninsula Medical Center |
| Lawrence J. Goldstein, MD |
| Endovascular surgery, minimally invasive surgery |
| 4 Financial Plaza |
| Napa, 707-266-7051 |
| Queen of the Valley Hospital |
| E. John Harris, MD |
| Aneurysm, endovascular surgery |
| 300 Pasteur Dr., Floor 3 |
| Stanford, 650-725-5227 |
| Stanford University Hospital & Clinics |
| John P. Loftus, MD |
| Aneurysm–aortic, carotid endarterectomy, peripheral vascular disease, endovascular surgery |
| 3443 Villa Ln., Ste. 5 |
| Napa, 707-226-2031 |
| Queen of the Valley Hospital |
| Daniel R. Nathanson, MD |
| Endovascular surgery, peripheral vascular disease, aortic surgery, aneurysm–abdominal & thoracic aortic |
| 1 Daniel Burnham Ct., Ste. 205C |
| San Francisco, 415-221-7056 |
| California Pacific Medical Center–Pacific Campus |
| Laura K. Pak, MD |
| Aneurysm–abdominal aortic, endovascular surgery, limb salvage, peripheral vascular disease |
| 1100 S. Eliseo Dr., Ste. 2A |
| Greenbrae, 415-464-5400 |
| Marin General Hospital |
| Lamont D. Paxton, MD |
| 13851 E. 14th St., Ste. 202 |
| San Leandro, 510-357-4006 |
| Eden Medical Center |
| James J. Zimmerman, MD |
| 2900 Whipple Ave., Ste. 225 |
| Redwood City, 650-366-0225 |
| Sequoia Hospital |
Top aging and health hacks 2-9-2018
|
|
| Signs of the preactive/ active phase of dying and medications for terminally ill | |
| View | |
| Nitric Oxide Dump Exercise with nose breathing to lower blood pressure and thin blood | |
| View | |
| Eggplant and apple cider vinegar for skin cancer | |
| View | |
| Home page / Archives | |
| View | |
| Can Gout be cured permanently? | |
| View | |
| Elon Musk, from South Africa, was an immigrant | |
| View | |
| Philippines Coconut Wine -Tuba | |
| View | |
| Non pasteurized beers have more health benefits | |
| View | |
| DMSO, hydrogen peroxide and Vit C fight cancer cells | |
| View | |
| What’s a good analogy to explain the immune system? | |
| View | |
| MEDICATIONS TO AVOID that worse PD (Parkinson’s disease) | |
| View | |
| Foods to eat and avoid when you have Gout and leg pains | |
| View | |
| Aphrodisiac foods | |
| View | |
| Nurture is every influence from without that affects man after his birth | |
| View | |
| Eat protein-rich food when drinking alcohol to protect your stomach | |
| View | |
| Anti-aging and Parkinson/Alzheimer’s prevention: Enzymes and apple cider vinegar | |
| View | |
| Avoid chronic bronchitis with green apple, onions, garlic, vinegar and rest | |
| View | |
| Good genes when selecting a partner | |
| View | |
| Nurture is every influence from without that affects man after his birth | |
| View | |
| 4 | |
| Conor James Lamb – Pennsylvania’s 18th congressional district | |
| View | |
| 4 | |
| Mike Pence involvement in Russia scandal | |
| View | |
| 4 | |
| Surviving prostate cancer by Dr Mercola | |
| View | |
| 4 | |
| Increase the body’s oxygen carrying capacity with exercise, EPO and whole foods | |
| View | |
| 4 | |
| Zinc and lemongrass for skin health issues | |
| View | |
| 4 | |
| Restless Legs Syndrome in Alzheimer’s and Parkinson’s Disease | |
| View | |
| 3 | |
| Skilled Nursing Facilities in the Bay area | |
| View | |
| 3 | |
| Top aging and health hacks 2-8-2018 | |
| View | |
| 3 | |
| Good genes when selecting a partner | |
| View | |
| 3 | |
| Spices that boost testosterone | |
| View | |
| 3 | |
| Can balsamic vinegar help with gout? | |
| View | |
| 3 | |
| Palo Alto Housing Work Plan | |
| View | |
| 2 | |
| Sovaldi , for Hepatitis C, is $483 in India and $84,000 in the USA | |
| View | |
| 2 | |
| Prostate cancer, Dr Mercola | |
| View | |
| 2 | |
| Fatigue and Red (bloodshot) eyes from WebMD | |
| View | |
| 2 | |
| Detox your lungs from air pollution and metal toxins and for early lung cancer | |
| View | |
| 2 | |
| Nitric Oxide for strong blood vessels’ cells , up with exercise, melons, cucumber, Vit C, E, amino acid – L-arginine, L-citrulline | |
| View | |
| 2 | |
| Weird Facts about Tall and Short People by Lisa Collier Cool | |
| View | |
| 2 | |
| Gout, Dementia, Chelation Therapy | |
| View | |
| 2 | |
| Liver cleanse to help your vision and memory | |
| View | |
| 2 | |
| Thyme herb for toe fungus (guava and comfrey leaves and others) | |
| View | |
| 2 | |
| Infected water from animal manure, prion disease and Parkinson | |
| View | |
| 2 | |
| Cash flow analysis worksheet template | |
| View | |
| 2 | |
| Be brave. Be an innovator. And be the change yourself. | |
| View | |
| 2 | |
| Dr Mercola’s Diverticulitis diet | |
| View | |
| 2 | |
| Iodine prevents cancer growth; up avocado and reduce caffeine intake to prevent Thyroid cancer | |
| View | |
| 2 | |
| Chest pain, flu and fever | |
| View | |
| 2 | |
| Fight VIRUS with Enzymes from pineapple and papaya, baking soda, alkaline food, calcium and magnesium from whole foods | |
| View | |
| 2 | |
| Gastroparesis, Betain HCL, diabetes and stomach health | |
| View | |
| 2 | |
| Dr Mercola’s Diverticulitis diet | |
| View | |
| 2 | |
| FOXO3, a gene linked to intelligence and involved in insulin signalling that might trigger apoptosis | |
| View | |
| 2 | |
| Your complete DNA sequence will help shape the future of medicine | |
| View | |
| 2 | |
| Shingles Natural Treatments | |
| View | |
| 2 | |
| Intestinal disorders , herbs and nutrition | |
| View | |
| 1 | |
| Growth hormone DHEA increases libido/anti-aging | |
| View | |
| 1 | |
| Stomach ulcers root causes | |
| View | |
| 1 | |
| Parkinson and Exercises | |
| View | |
| 1 | |
| The World’s smoking population | |
| View | |
| 1 | |
| TP53 gene affects tumor suppression | |
| View | |
| 1 | |
| Goat’s milk is next to breastmilk | |
| View | |
| 1 | |
| Magnesium for Parkinson’s and other chronic disorders and for anti-aging | |
| View | |
| 1 | |
| Chlorine rich foods are cleansing (avocado, coconut, onions, parsnips) | |
| View | |
| 1 | |
| Pineapple, celery, carrots and Arthritis | |
| View | |
| 1 | |
| Blindness and Amnesia cure using Optogenetics | |
| View | |
| 1 | |
| Digestive enzymes help in healing fractures, preventing kidney stones and heart disease and more | |
| View | |
| 1 | |
| Cardio-based body weight exercises | |
| View | |
| 1 | |
| Restore your vision naturally y Dr. Mercola | |
| View | |
| 1 | |
| MindMaze receives FDA clearance to bring VR rehab platform to the US | |
| View | |
| 1 | |
| Cooked your greens rich in oxalates to prevent kidney stones | |
| View | |
| 1 | |
| Altered Lipid Metabolism in Brain Injury and Disorders | |
| View | |
| 1 | |
| Alzheimer’s Association’s 19th Annual Updates on Dementia Conference | |
| View | |
| 1 | |
| How does a CBC test for a leukemia patient usually look like? | |
| View | |
| 1 | |
| If You Get the Chills From Music, you have ability to feel intense emotions | |
| View | |
| 1 | |
| Mike Pence Implicated in Treason Scandal | |
| View | |
| 1 | |
| Anti aging plants and herbs | |
| View | |
| 1 | |
| Does drinking warm water reduce cholesterol? | |
| View | |
| 1 | |
| Taste Of Beer Triggers Release Of Dopamine, happy neurotransmitter ; Cocaine bullies dopamine; MAO affects dopamine levels | |
| View | |
| 1 | |
| Hunched posture in Dementia and Parkinsons | |
| View | |
| 1 | |
| How close are we to finding a cure for pulmonary hypertension? | |
| View | |
| 1 | |
| Gout, Dementia, Chelation Therapy | |
| View | |
| 1 | |
| No grains, dairy, processed foods and sugars for active Crohn’s disease and ulcerative colitis | |
| View | |
| 1 | |
| How important is the thymus gland in keeping your body free from diseases? | |
| View | |
| 1 | |
| Vagus nerve stimulation thru breathing, laughs and yoga | |
| View | |
| 1 | |
| Anti-aging Vitamin B3, Niacin | |
| View | |
| 1 | |
| Suicide deaths of active-duty US military and omega-3 fatty-acid status | |
| View | |
| 1 | |
| Massage oil of fresh ginger and coconut oil relieves joint pain | |
| View | |
| 1 | |
| Top health and aging hacks 1-8-2018 | |
| View | |
| 1 | |
| Make your own alkaline water to kill any virus growth | |
| View | |
| 1 | |
| Dr Perlmutter on ADHD and diet, ketosis and Parkinsons, and Dementia | |
| View | |
| 1 | |
| Nominate your best doctor in the bay area | |
| View | |
| 1 | |
| Caregivers $15 – 32 per hr for senior non-medical home care in the bay area | |
| View | |
| 1 | |
| Caregivers $15 – 32 per hr for senior non-medical home care in the bay area | |
| View | |
| 1 | |
| Fungus , raw carrots and prostate cancer | |
| View | |
| 1 | |
| Fresno VA Medical Center’s Nurse of the Year | |
| View | |
| 1 | |
| New York Times 8-23-2107 | |
| View | |
| 1 | |
| Vitamin A deficient lung – COPD – hospice in home senior care | |
| View | |
| 1 | |
| Aphrodisiac foods | |
| View | |
| 1 | |
| Coconut and cinnamon for Alzheimer’s disease | |
| View | |
| 1 | |
| Knowing more about our brain for longevity | |
| View | |
| 1 | |
| Robert Mueller III stood up against corruption | |
| View | |
| 1 | |
| Top health and aging hacks 1-9-18 | |
| View | |
| 1 | |
| Tanglad or lemongrass to help lower blood pressure | |
| View | |
| 1 | |
| Low bar set by media for con man | |
| View | |
| 1 | |
| House cleaner, cook, driver and caregiver – takes a village to do in home health care | |
| View | |
| 1 | |
| Police then Funeral Homes before body is removed from the house | |
| View | |
| 1 | |
| Police then Funeral Homes before body is removed from the house | |
| View | |
| 1 | |
| Truth and corruption in WH | |
| View | |
| 1 | |
| ‘Category 5 hurricane’: White House under siege by Trump Jr.’s Russia revelations | |
| View | |
| 1 | |
| Hunched posture in Dementia and Parkinsons | |
| View | |
| 1 | |
| Low back pain in older adults | |
| View | |
| 1 | |
| Cough remedies from Dr Mercola | |
| View | |
| 1 | |
| What is Precision, predictive and Personalize Medicine vs patient-centered care | |
| View | |
| 1 | |
| Neck pain and MTHFR gene , folate , methionine | |
| View | |
| 1 | |
| Why New Antidepressant Brintellix May Be a Killer | |
| View | |
| 1 | |
| Atopic dermatitis and psoriasis by Dr Mercola | |
| View | |
| 1 | |
| When will Souvenaid become available in Canada and US to treat Alzheimer’s Disease? | |
| View | |
| 1 | |
| Infected water from animal manure, prion disease and Parkinson |
Infected water from animal manure, prion disease and Parkinson
Infected water from animal manure, prion disease and Parkinson
Prion diseases and their transmission properties
| Affected animal(s) | Disease |
|---|---|
| sheep, goat | Scrapie[43] |
| cattle | Bovine spongiform encephalopathy (BSE), mad cow disease[43] |
| mink[43] | Transmissible mink encephalopathy (TME) |
| white-tailed deer, elk, mule deer, moose[43] | Chronic wasting disease (CWD) |
| cat[43] | Feline spongiform encephalopathy (FSE) |
| nyala, oryx, greater kudu[43] | Exotic ungulate encephalopathy (EUE) |
| ostrich[44] | Spongiform encephalopathy (Has not been shown to be transmissible.) |
| human | Creutzfeldt–Jakob disease (CJD)[43] |
| Iatrogenic Creutzfeldt–Jakob disease (iCJD) | |
| Variant Creutzfeldt–Jakob disease (vCJD) | |
| Familial Creutzfeldt–Jakob disease (fCJD) | |
| Sporadic Creutzfeldt–Jakob disease (sCJD) | |
| Gerstmann–Sträussler–Scheinker syndrome (GSS)[43] | |
| Fatal familial insomnia (FFI)[45] | |
| Kuru[43] | |
| Familial spongiform encephalopathy[46] | |
| Multiple System Atrophy (MSA): Not a TSE and is not by typical prions Prp/PrPSc but by a misfolded α-Synuclein.[47] |
Until 2015 all known mammalian prion diseases were considered to be caused by the prion protein, PrP; in 2015 Multiple System Atrophy was found to be likely caused by a new prion, the misfolded form of a protein called alpha-synuclein.[4]The endogenous, properly folded form of the prion protein is denoted PrPC (for Common or Cellular), whereas the disease-linked, misfolded form is denoted PrPSc (for Scrapie), after one of the diseases first linked to prions and neurodegeneration.)[22][48] The precise structure of the prion is not known, though they can be formed by combining PrPC, polyadenylic acid, and lipids in a protein misfolding cyclic amplification (PMCA) reaction.[49] Proteins showing prion-type behavior are also found in some fungi, which has been useful in helping to understand mammalian prions. Fungal prions do not appear to cause disease in their hosts.[50]
Prions cause neurodegenerative disease by aggregating extracellularly within the central nervous system to form plaques known as amyloid, which disrupt the normal tissue structure. This disruption is characterized by “holes” in the tissue with resultant spongy architecture due to the vacuole formation in the neurons.[51]Other histological changes include astrogliosis and the absence of an inflammatory reaction.[52] While the incubation period for prion diseases is relatively long (5 to 20 years), once symptoms appear the disease progresses rapidly, leading to brain damage and death.[53] Neurodegenerative symptoms can include convulsions, dementia, ataxia (balance and coordination dysfunction), and behavioural or personality changes.
All known prion diseases, collectively called transmissible spongiform encephalopathies (TSEs), are untreatable and fatal.[54] However, a vaccine developed in mice may provide insight into providing a vaccine to resist prion infections in humans.[55] Additionally, in 2006 scientists announced that they had genetically engineered cattle lacking a necessary gene for prion production – thus theoretically making them immune to BSE,[56] building on research indicating that mice lacking normally occurring prion protein are resistant to infection by scrapie prion protein.[57] In 2013, a study revealed that 1 in 2,000 people in the United Kingdom might harbour the infectious prion protein that causes vCJD.[58]
Many different mammalian species can be affected by prion diseases, as the prion protein (PrP) is very similar in all mammals.[59] Due to small differences in PrP between different species it is unusual for a prion disease to transmit from one species to another. The human prion disease variant Creutzfeldt–Jakob disease, however, is believed to be caused by a prion that typically infects cattle, causing Bovine spongiform encephalopathy and is transmitted through infected meat.[60]
Transmission
It has been recognized that prion diseases can arise in three different ways: acquired, familial, or sporadic.[61] It is often assumed that the diseased form directly interacts with the normal form to make it rearrange its structure. One idea, the “Protein X” hypothesis, is that an as-yet unidentified cellular protein (Protein X) enables the conversion of PrPC to PrPSc by bringing a molecule of each of the two together into a complex.[62]
Current research suggests that the primary method of infection in animals is through ingestion. It is thought that prions may be deposited in the environment through the remains of dead animals and via urine, saliva, and other body fluids. They may then linger in the soil by binding to clay and other minerals.[63]
A University of California research team, led by Nobel Prize winner Stanley Prusiner, has provided evidence for the theory that infection can occur from prions in manure.[64] And, since manure is present in many areas surrounding water reservoirs, as well as used on many crop fields, it raises the possibility of widespread transmission. It was reported in January 2011 that researchers had discovered prions spreading through airborne transmission on aerosol particles, in an animal testingexperiment focusing on scrapie infection in laboratory mice.[65] Preliminary evidence supporting the notion that prions can be transmitted through use of urine-derived human menopausal gonadotropin, administered for the treatment of infertility, was published in 2011.[66]
Prions in plants
In 2015, researchers at The University of Texas Health Science Center at Houston found that plants can be a vector for prions. When researchers fed hamsters grass that grew on ground where a deer that died with chronic wasting disease (CWD) was buried, the hamsters became ill with CWD, suggesting that prions can bind to plants, which then take them up into the leaf and stem structure, where they can be eaten by herbivores, thus completing the cycle. It is thus possible that there is a progressively accumulating number of prions in the environment.[67][68]
Sterilization
Infectious particles possessing nucleic acid are dependent upon it to direct their continued replication. Prions, however, are infectious by their effect on normal versions of the protein. Sterilizing prions, therefore, requires the denaturation of the protein to a state in which the molecule is no longer able to induce the abnormal folding of normal proteins. In general, prions are quite resistant to proteases, heat, ionizing radiation, and formaldehyde treatments,[69] although their infectivity can be reduced by such treatments. Effective prion decontamination relies upon protein hydrolysis or reduction or destruction of protein tertiary structure. Examples include sodium hypochlorite, sodium hydroxide, and strongly acidic detergents such as LpH.[70] 134 °C (274 °F) for 18 minutes in a pressurized steam autoclave has been found to be somewhat effective in deactivating the agent of disease.[71][72] Ozone sterilization is currently being studied as a potential method for prion denaturation and deactivation.[73] Renaturation of a completely denatured prion to infectious status has not yet been achieved; however, partially denatured prions can be renatured to an infective status under certain artificial conditions.[74]
The World Health Organization recommends any of the following three procedures for the sterilization of all heat-resistant surgical instruments to ensure that they are not contaminated with prions:
- Immerse in 1N sodium hydroxide and place in a gravity-displacement autoclave at 121 °C for 30 minutes; clean; rinse in water; and then perform routine sterilization processes.
- Immerse in 1N sodium hypochlorite (20,000 parts per million available chlorine) for 1 hour; transfer instruments to water; heat in a gravity-displacement autoclave at 121 °C for 1 hour; clean; and then perform routine sterilization processes.
- Immerse in 1N sodium hydroxide or sodium hypochlorite (20,000 parts per million available chlorine) for 1 hour; remove and rinse in water, then transfer to an open pan and heat in a gravity-displacement (121 °C) or in a porous-load (134 °C) autoclave for 1 hour; clean; and then perform routine sterilization processes.[75]
Prion-like domains
While PrP is considered the only mammalian prion, prion-like domains have been found in a variety of other mammalian proteins. Some of these proteins have been implicated in the ontogeny of age-related neurodegenerative disorders such as amyotrophic lateral sclerosis (ALS, known as Motor Neurone Disease outside the US), frontotemporal lobar degeneration with ubiquitin-positive inclusions (FTLD-U), Alzheimer’s disease, and Huntington’s disease,[76] as well as some forms of Systemic Amyloidosis including AA (Secondary) Amyloidosis that develops in humans and animals with inflammatory and infectious diseases such as Tuberculosis, Crohn’s disease, Rheumatoid arthritis, and HIV AIDS. AA amyloidosis, like prion disease, may be transmissible.[77] This has given rise to the ‘prion paradigm’, where otherwise harmless proteins can be converted to a pathogenic form by a small number of misfolded, nucleating proteins.[78]
The definition of a prion-like domain arises from the study of fungal prions. In yeast, prionogenic proteins have a portable prion domain that is both necessary and sufficient for self-templating and protein aggregation. This has been shown by attaching the prion domain to a reporter protein, which then aggregates like a known prion. Similarly, removing the prion domain from a fungal prion protein inhibits prionogenesis. This modular view of prion behaviour has led to the hypothesis that similar prion domains are present in animal proteins, in addition to PrP.[76] These fungal prion domains have several characteristic sequence features. They are typically enriched in asparagine, glutamine, tyrosine and glycine residues, with an asparagine bias being particularly conducive to the aggregative property of prions. Historically, prionogenesis has been seen as independent of sequence and only dependent on relative residue content. However, this has been shown to be false, with the spacing of prolines and charged residues having been shown to be critical in amyloid formation.[5]
Bioinformatic screens have predicted that over 250 human proteins contain prion-like domains (PrLD). These domains are hypothesized to have the same transmissible, amyloidogenic properties of PrP and known fungal proteins. As in yeast, proteins involved in gene expression and RNA binding seem to be particularly enriched in PrLD’s, compared to other classes of protein. In particular, 29 of the known 210 proteins with an RNA recognition motif also have a putative prion domain. Meanwhile, several of these RNA-binding proteins have been independently identified as pathogenic in cases of ALS, FTLD-U, Alzheimer’s disease, and Huntington’s disease.[79]
Role in neurodegenerative disease
The pathogenicity of prions and proteins with prion-like domains arises from their self-templating ability and the resulting exponential growth of amyloid fibrils. The presence of amyloid fibrils in patients with degenerative diseases has been well documented. These amyloid fibrils are seen as the result of pathogenic proteins that self-propagate and form highly stable, non-functional aggregates.[79] While this does not necessarily imply a causal relationship between amyloid and degenerative diseases, the toxicity of certain amyloid forms and the overproduction of amyloid in familial cases of degenerative disorders supports the idea that amyloid formation is generally toxic.
Specifically, aggregation of TDP-43, an RNA-binding protein, has been found in ALS/MND patients, and mutations in the genes coding for these proteins have been identified in familial cases of ALS/MND. These mutations promote the misfolding of the proteins into a prion-like conformation. The misfolded form of TDP-43 forms cytoplasmic inclusions in afflicted neurons, and is found depleted in the nucleus. In addition to ALS/MND and FTLD-U, TDP-43 pathology is a feature of many cases of Alzheimer’s disease, Parkinson’s disease and Huntington’s disease. The misfolding of TDP-43 is largely directed by its prion-like domain. This domain is inherently prone to misfolding, while pathological mutations in TDP-43 have been found to increase this propensity to misfold, explaining the presence of these mutations in familial cases of ALS/MND. As in yeast, the prion-like domain of TDP-43 has been shown to be both necessary and sufficient for protein misfolding and aggregation.[76]
Similarly, pathogenic mutations have been identified in the prion-like domains of heterogeneous nuclear riboproteins hnRNPA2B1 and hnRNPA1 in familial cases of muscle, brain, bone and motor neuron degeneration. The wild-type form of all of these proteins show a tendency to self-assemble into amyloid fibrils, while the pathogenic mutations exacerbate this behaviour and lead to excess accumulation.[80]
Fungi
Fungal proteins exhibiting templated conformational change were discovered in the yeast Saccharomyces cerevisiae by Reed Wickner in the early 1990s. For their mechanistic similarity to mammalian prions, they were termed yeast prions. Subsequent to this, a prion has also been found in the fungus Podospora anserina. These prions behave similarly to PrP, but, in general, are nontoxic to their hosts. Susan Lindquist‘s group at the Whitehead Institute has argued some of the fungal prions are not associated with any disease state, but may have a useful role; however, researchers at the NIH have also provided arguments suggesting that fungal prions could be considered a diseased state.[81] There is mounting evidence that fungal proteins have evolved specific functions that are beneficial to the microorganism that enhance their ability to adapt to their diverse environments.[82]
As of 2012, there are eight known prion proteins in fungi, seven in Saccharomyces cerevisiae (Sup35, Rnq1, Ure2, Swi1, Mot3, Cyc8, and Mod5) and one in Podospora anserina (HET-s).[contradictory] The article that reported the discovery of a prion form, the Mca1 protein, was retracted due to the fact that the data could not be reproduced.[83] Notably, most of the fungal prions are based on glutamine/asparagine-rich sequences, with the exception of HET-s and Mod5.
Research into fungal prions has given strong support to the protein-only concept, since purified protein extracted from cells with a prion state has been demonstrated to convert the normal form of the protein into a misfolded form in vitro, and in the process, preserve the information corresponding to different strains of the prion state. It has also shed some light on prion domains, which are regions in a protein that promote the conversion into a prion. Fungal prions have helped to suggest mechanisms of conversion that may apply to all prions, though fungal prions appear distinct from infectious mammalian prions in the lack of cofactor required for propagation. The characteristic prion domains may vary between species—e.g., characteristic fungal prion domains are not found in mammalian prions.
Connie’s comments: I have a client with Parkinson, Dementia and Lew Body diseases who likes to drink raw milk. Do drink pasteurized milk and milk products. I do not drink milk.
Suicide deaths of active-duty US military and omega-3 fatty-acid status
Suicide deaths of active-duty US military and omega-3 fatty-acid status: a case-control comparison.
The recent escalation of US military suicide deaths to record numbers has been a sentinel for impaired force efficacy and has accelerated the search for reversible risk factors.
OBJECTIVE:
To determine whether deficiencies of neuroactive, highly unsaturated omega-3 essential fatty acids (n-3 HUFAs), in particular docosahexaenoic acid (DHA), are associated with increased risk of suicide death among a large random sample of active-duty US military.
METHOD:
In this retrospective case-control study, serum fatty acids were quantified as a percentage of total fatty acids among US military suicide deaths (n = 800) and controls (n = 800) matched for age, date of collection of sera, sex, rank, and year of incident. Participants were active-duty US military personnel (2002-2008). For cases, age at death ranged from 17-59 years (mean = 27.3 years, SD = 7.3 years). Outcome measures included death by suicide, postdeployment health assessment questionnaire (Department of Defense Form 2796), and ICD-9 mental health diagnosis data.
RESULTS:
Risk of suicide death was 14% higher per SD of lower DHA percentage (OR = 1.14; 95% CI, 1.02-1.27; P < .03) in adjusted logistic regressions. Among men, risk of suicide death was 62% greater with low serum DHA status (adjusted OR = 1.62; 95% CI, 1.12-2.34; P < .01, comparing DHA below 1.75% [n = 1,389] to DHA of 1.75% and above [n = 141]). Risk of suicide death was 52% greater in those who reported having seen wounded, dead, or killed coalition personnel (OR = 1.52; 95% CI, 1.11-2.09; P < .01).
CONCLUSION:
This US military population had a very low and narrow range of n-3 HUFA status. Although these data suggest that low serum DHA may be a risk factor for suicide, well-designed intervention trials are needed to evaluate causality.
Elon Musk, from South Africa, was an immigrant
As the issue of illegal immigration continued to pop in 2016 presidential election debates, a meme began circulating on Facebook claiming that Elon Musk, the CEO of Tesla Motors, was once an undocumented immigrant:
I am Elon Musk. I was an ILLEGAL immigrant and if Mr. Trump and some of you had it your way, I would’ve been kicked out of the USA and never founded Zip2, PayPal, Tesla Motors, SpaceX, Solar City. I wouldn’t have changed the world and employed thousands of Americans and grown your economy.
Musk indeed entered the United States an immigrant, but there is little evidence that he was ever in the U.S. without documentation. According to an Esquire profile of Musk, he was born in South Africa and obtained Canadian citizenship through his mother in 1989:
Elon made his move after he graduated high school. Though he already felt like an American, he’d done research and concluded that it would be easier to obtain American citizenship as a Canadian immigrant rather than as a South African one. His mother was from Canada. Most of her family still lived there.
Musk first came to the United States in 1992 after transferring from Queen’s University in Ontario to the University of Pennsylvania. He said in an interview his decision attend school in the United States was based partly on his desire to get an education, but also because the move would allow him to remain in the country afterwards:
In my case I had to (attend college), otherwise I’d get kicked out of the country. So, that was important.
I came out to Silicon Valley to do a PhD at Stanford, in applied physics and material science to work on ultracapacitors for use in electric cars. And that’s what I was going to do, and then I decided to put that on hold to start a company. But since I already had my undergrad, I could then get a H-1B visa and that kinda thing. So the H-1B visa requires a degree. But other than that, if that wasn’t the case, I probably would’ve stopped education sooner.
Musk moved to California in 1995, and in 2002 he officially became an American citizen:
Ten years ago — ten years after his arrival in the New World — Elon Musk took the oath of American citizenship with thirty-five hundred other immigrants at the Pomona Fairplex, in a ceremony he calls “actually very moving.”
The meme likely originated with an appearance Musk made on The Dinner Program. While Musk’s brother Kimbal once joked that they had been “illegal immigrants,” Elon said that this was a “gray area” (and indeed, American immigration policy in all its complexity contains a good number of “gray areas”) and that he considers himself a legal immigrant
Nurture is every influence from without that affects man after his birth
Nurture is every influence from without that affects man after his birth
Summary: A new study reveals a diverse array of genetic changes that occur in the brain following sensory experiences.
Source: Harvard.
“Nature and nurture is a convenient jingle of words, for it separates under two distinct heads the innumerable elements of which personality is composed. Nature is all that a man brings with himself into the world; nurture is every influence from without that affects him after his birth.” – Francis Galton, cousin of Charles Darwin, 1874.
Is it nature or nurture that ultimately shapes a human? Are actions and behaviors a result of genes or environment? Variations of these questions have been explored by countless philosophers and scientists across millennia. Yet, as biologists continue to better understand the mechanisms that underlie brain function, it is increasingly apparent that this long-debated dichotomy may be no dichotomy at all.
In a study published in Nature Neuroscience on Jan. 21, neuroscientists and systems biologists from Harvard Medical School reveal just how inexorably interwoven nature and nurture are in the mouse brain. Using novel technologies developed at HMS, the team looked at how a single sensory experience affects gene expression in the brain by analyzing more than 114,000 individual cells in the mouse visual cortex before and after exposure to light.
Their findings revealed a dramatic and diverse landscape of gene expression changes across all cell types, involving 611 different genes, many linked to neural connectivity and the brain’s ability to rewire itself to learn and adapt.
The results offer insights into how bursts of neuronal activity that last only milliseconds trigger lasting changes in the brain, and open new fields of exploration for efforts to understand how the brain works.
“What we found is, in a sense, amazing. In response to visual stimulation, virtually every cell in the visual cortex is responding in a different way,” said co-senior author Michael Greenberg, the Nathan Marsh Pusey Professor of Neurobiology and chair of the Department of Neurobiology at HMS.
“This in essence addresses the long-asked question about nature and nurture: Is it genes or environment? It’s both, and this is how they come together,” he said.
One out of many
Neuroscientists have known that stimuli–sensory experiences such as touch or sound, metabolic changes, injury and other environmental experiences–can trigger the activation of genetic programs within the brain.
Composed of a vast array of different cells, the brain depends on a complex orchestra of cellular functions to carry out its tasks. Scientists have long sought to understand how individual cells respond to various stimuli. However, due to technological limitations, previous genetic studies largely focused on mixed populations of cells, obscuring critical nuances in cellular behavior.
To build a more comprehensive picture, Greenberg teamed with co-corresponding author Bernardo Sabatini, the Alice and Rodman W. Moorhead III Professor of Neurobiology at HMS, and Allon Klein, assistant professor of systems biology at HMS.
Spearheaded by co-lead authors Sinisa Hrvatin, a postdoctoral fellow in the Greenberg lab, Daniel Hochbaum, a postdoctoral fellow in the Sabatini lab and M. Aurel Nagy, an MD-PhD student in the Greenberg lab, the researchers first housed mice in complete darkness to quiet the visual cortex, the area of the brain that controls vision.
They then exposed the mice to light and studied how it affected genes within the brain. Using technology developed by the Klein lab known as inDrops, they tracked which genes got turned on or off in tens of thousands of individual cells before and after light exposure.
The team found significant changes in gene expression after light exposure in all cell types in the visual cortex–both neurons and, unexpectedly, nonneuronal cells such as astrocytes, macrophages and muscle cells that line blood vessels in the brain.
Roughly 50 to 70 percent of excitatory neurons, for example, exhibited changes regardless of their location or function. Remarkably, the authors said, a large proportion of non-neuronal cells–almost half of all astrocytes, for example–also exhibited changes.
The team identified thousands of genes with altered expression patterns after light exposure, and 611 genes that had at least two-fold increases or decreases.
Many of these genes have been previously linked to structural remodeling in the brain, suggesting that virtually the entire visual cortex, including the vasculature and muscle cell types, may undergo genetically controlled rewiring in response to a sensory experience.
There has been some controversy among neuroscientists over whether gene expression could functionally control plasticity or connectivity between neurons.
“I think our study strongly suggests that this is the case, and that each cell has a unique genetic program that’s tailored to the function of a given cell within a neural circuit,” Greenberg said.
Question goldmine
These findings open a wide range of avenues for further study, the authors said. For example, how genetic programs affect the function of specific cell types, how they vary early or later in life and how dysfunction in these programs might contribute to disease, all of which could help scientists learn more about the fundamental workings of the brain.
“Experience and environmental stimuli appear to almost constantly affect gene expression and function throughout the brain. This may help us to understand how processes such as learning and memory formation, which require long-term changes in the brain, arise from the short bursts of electrical activity through which neurons signal to each other,” Greenberg said.
One especially interesting area of inquiry, according to Greenberg, includes the regulatory elements that control the expression of genes in response to sensory experience. In a paper published earlier this year in Molecular Cell, he and his team explored the activity of the FOS/JUN protein complex, which is expressed across many different cell types in the brain but appears to regulate unique programs in each different cell type.
Identifying the regulatory elements that control gene expression is critical because they may account for differences in brain function from one human to another, and may also underlie disorders such as autism, schizophrenia and bipolar disease, the researchers said.
“We’re sitting on a goldmine of questions that can help us better understand how the brain works,” Greenberg said. “And there is a whole field of exploration waiting to be tapped.”
Additional authors on the study include Marcelo Cicconet, Keiramarie Robertson, Lucas Cheadle, Rapolas Zilionis, Alex Ratner and Rebeca Borges-Monroy.
Funding: This work was supported by the National Institutes of Health (R01NS028829, R01NS046579, T32GM007753, R33CA212697, 5T32AG000222-23), F. Hoffmann-La Roche Ltd., the William F. Milton Fund, a Burroughs Wellcome Fund Career Award and an Edward J. Mallinckrodt Scholarship.
Source: Ekaterina Pesheva – Harvard
Publisher: Organized by NeuroscienceNews.com.
Image Source: NeuroscienceNews.com image is credited to Lichtman Lab, Harvard University.
Original Research: Abstract in Nature Neuroscience.
DOI:10.1038/s41593-017-0029-5
<http://neurosciencenews.com/genetic-nature-experience-8455/>.
Abstract
Single-cell analysis of experience-dependent transcriptomic states in the mouse visual cortex
Activity-dependent transcriptional responses shape cortical function. However, a comprehensive understanding of the diversity of these responses across the full range of cortical cell types, and how these changes contribute to neuronal plasticity and disease, is lacking. To investigate the breadth of transcriptional changes that occur across cell types in the mouse visual cortex after exposure to light, we applied high-throughput single-cell RNA sequencing. We identified significant and divergent transcriptional responses to stimulation in each of the 30 cell types characterized, thus revealing 611 stimulus-responsive genes. Excitatory pyramidal neurons exhibited inter- and intralaminar heterogeneity in the induction of stimulus-responsive genes. Non-neuronal cells showed clear transcriptional responses that may regulate experience-dependent changes in neurovascular coupling and myelination. Together, these results reveal the dynamic landscape of the stimulus-dependent transcriptional changes occurring across cell types in the visual cortex; these changes are probably critical for cortical function and may be sites of deregulation in developmental brain disorders.
Connie’s comments:
I massaged my babies after birth before each bath and even up to now when they are sick. I train all caregivers to massage home-bound older adults or seniors needing 24/7 care.

Zinc and lemongrass for skin health issues
Mum thought her ‘melting skin’ baby would be better off dead – but her …
Aug 6, 2015 – Instead we used thin cotton sheets. “He was most comfortable … Following her mother’s instinct, Stephanie stopped applying topical steroids and began to develop her own homeopathic balms. Having made candles in … A blend of lemongrass and zinc, applied under gauze, worked best. She said: “As time …
blend of lemongrass and zinc for lesions – Inspire
LemonGrass Balm $10: https://www.amazon.com/Lemongrass-natural-Good-Earth-Beauty/dp/B00LVCF4ZW/r ef=pd_sim_75_2?ie=UTF8&psc=1&refRID=6G3K2BRX26XMP6RC4XFA Maybe mix LemonGrass Balm w/ ZnO (Zinc Oxide) …Instead of the damaging Steroid Topicals ! Edited September 30 …
Mom Discovers That Treating Her Son With Topical Steroid Was
Aug 20, 2015 – Red raw skin, flaking off and oozing.” Smith decided to stop using topical steroids to treat her son, instead experimenting with homemade, homeopathic balms she concocted using her experience with candle-making. It was a blend of lemongrass and zinc, applied under gauze, that finally made a difference.
// Our Lemongrass and Zinc balm combo… – The Home Apothecary …
Our Lemongrass and Zinc balm combo is our top seller on our Etsy shop! These two balms were originally created for our baby son, Isaiah Quinn, as he journeyed through Topical Steroid Withdrawal. Now, (over 6,000 sales later!!!) they are used for eczema and skin conditions of all types, and many of our 500+ shop …
Kline’s road from out of control eczema to topical steroid withdrawal to …
Apr 5, 2014 – I was saving the balm for Kline and I tried his vanicream (KLINE COULD NOT TOLERATE THE VANICREAM, HE SCREAMED BLOODY MURDER..and begged me to put the lemongrass balm on him instead….the vanicream also made him have an all over body rash.) on me and it dried my skin right up, …
Mom Realizes What Doctors Have Been Treating Her Son With is …
Aug 7, 2015 – … instinct and stopped using steroids to treat Isaiah’s rashes. Instead, she started making her own homeopathic balms, experimenting with different formulations in the effort to find the most effective treatment. Image Credit: Isaiah Quinn Blog. Isaiah Quinn Blog. A combination oflemongrass and zinc seemed …
Zinc Oxide to Treat Eczema | LIVESTRONG.COM
Topical corticosteroids can treat lichenified eczema, or skin that has thickened and toughened because of chronic scratching. Your doctor may recommend applying bandages over the corticosteroidto boost absorption of the medicine into the skin. Bandages containing ichthammol paste and zinc paste also help decrease …
Homemade zinc cream for topical steroid withdrawal/eczema sufferers …
Disclaimer- Please patch test the lotion before using to ensure that you do not have an allergy to any ingredients …
Shingles Natural Treatment: Foods, Supplements & Oils to Help – Dr. Axe
#4 Vitamin B12 (1000-5000 mcg daily) Vitamin B12 helps promote faster recovery and reduced pain. #5Zinc (50 mg daily) Zinc supports immune function and has … then a doctor will likely recommend a topical shingles cream containing capsaicin, a topical numbing agent or even injections of steroids or local anesthetics.